EGFR-positive tumors: the issue of optimal therapy across several lines
FLAURA: OS with first-line osimertinib
In patients with advanced, EGFR-positive NSCLC, EGFR tyrosine kinase inhibitors (TKIs) represent the frontline treatment standard. Three generations of TKIs are widely available, but the ideal sequence is currently unknown. The phase III, double-blind, randomized FLAURA trial compared the third-generation EGFR TKI osimertinib with the first-generation agents gefitinib and erlotinib in the frontline setting. At the time of the primary analysis, which had shown a significant PFS benefit for osimertinib (18.9 vs. 10.2 months; HR, 0.46; p < 0.001), survival outcomes had not been mature yet [1]. Ramalingam et al. presented the final results for OS, which was defined as a key secondary endpoint of the study, at ESMO 2019 [2].
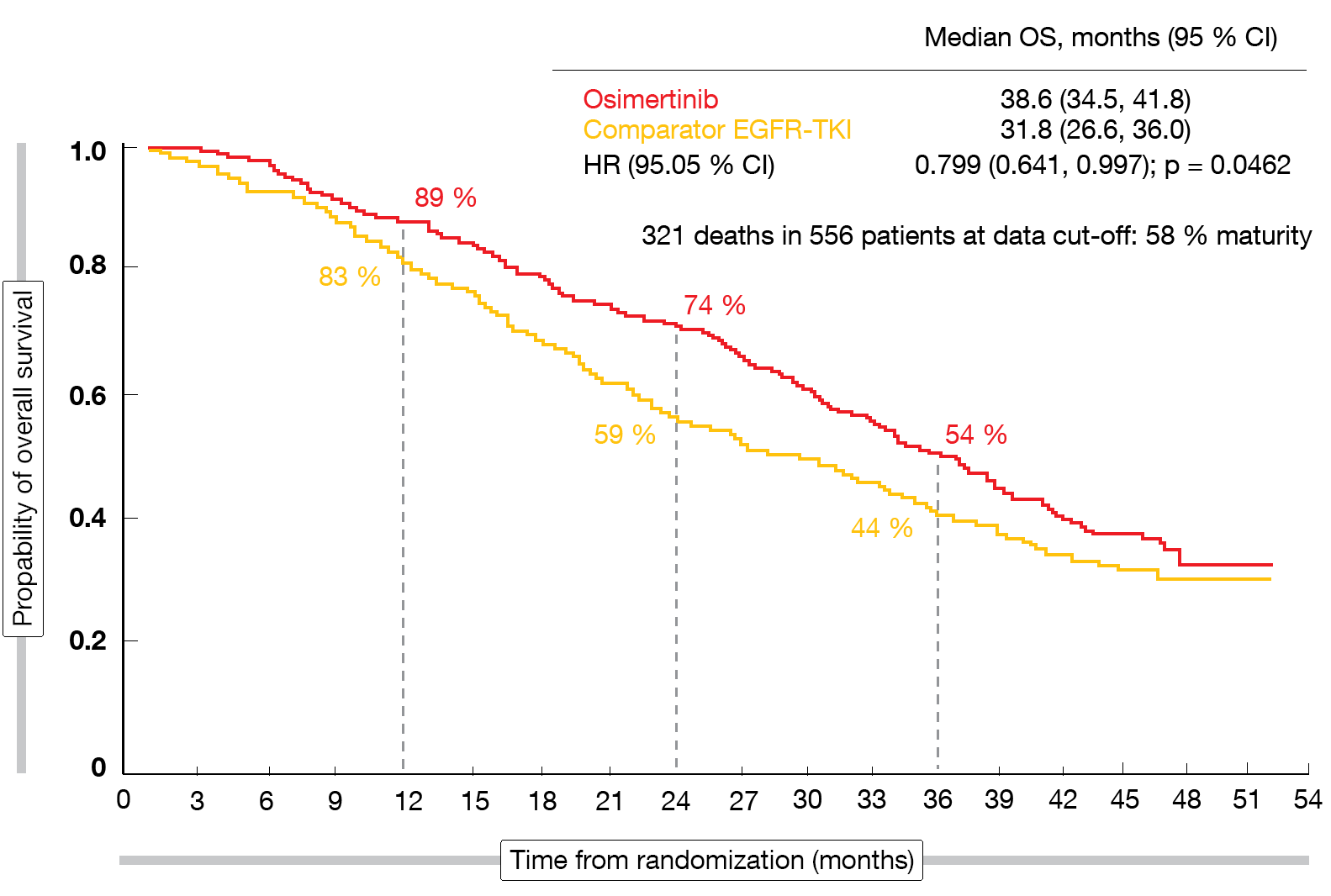
FLAURA demonstrated a statistically significant and clinically meaningful OS improvement with osimertinib compared to gefitinib or erlotinib (38.6 vs. 31.8 months; HR, 0.799; p = 0.0462; Figure 1). At 24 months, 74 % vs. 59 % of patients were alive; at 36 months, this applied to 54 % vs. 44 %. As OS was a secondary endpoint, the trial was not powered to assess OS effects in each subgroup. However, all patients derived OS benefit from the third-generation TKI treatment compared to the control arm, although the magnitude of benefit was greater in the non-Asian subgroup than in the Asian cohort. For Asian patients, the Kaplan Meier curves indicate a survival advantage throughout the first three years of the study. At 36 months, a high degree of censoring and a smaller number of events render interpretation difficult.
Figure 1: Final overall survival results for osimertinib vs. gefitinib or erlotinib in the FLAURA trial
Subsequent treatments
The duration of time to first subsequent therapy or death observed in the osimertinib arm was almost double that obtained with the comparator agents (25.5 vs. 13.7 months; HR, 0.478; p < 0.0001). At 36 months, 28 % vs. 9 % of patients remained on study treatment. Thirty percent in both trial arms were not able to receive any subsequent therapy, and the majority of these died after the onset of disease progression. In the osimertinib arm, 47 % of patients who experienced progression went on second-line anticancer treatment, which mainly consisted of cytotoxic chemotherapy (68 %). Sixty-five percent of those in the comparator arm received second-line treatment, with osimertinib being the most commonly prescribed agent (47 %). Chemotherapy was administered in 22 % in this group.
Despite prolonged exposure in the experimental arm of FLAURA that exceeded exposure in the comparator arm (20.7 vs. 11.5 months), osimertinib showed a favorable toxicity profile that was consistent with known findings. A comparatively smaller proportion of patients on third-generation TKI therapy developed possibly treatment-related grade ≥ 3 adverse events (18 % vs. 29 %). The authors noted that the final OS analysis of FLAURA reinforces osimertinib as the standard of care for frontline treatment of patients with EGFR-mutant advanced NSCLC. Osimertinib is the first EGFR TKI monotherapy to show a statistically significant OS benefit compared to another EGFR TKI.
Liquid monitoring of early signs of progression
An exploratory analysis of the FLAURA study investigated serial circulating tumor DNA (ctDNA) for the early molecular detection of progressive disease and resistance mechanisms [3]. Among 556 patients randomized in FLAURA, 122 were eligible for ctDNA analyses (42 and 80 in the osimertinib and comparator arms, respectively). C797S and T790M were the only resistance mutations tested for.
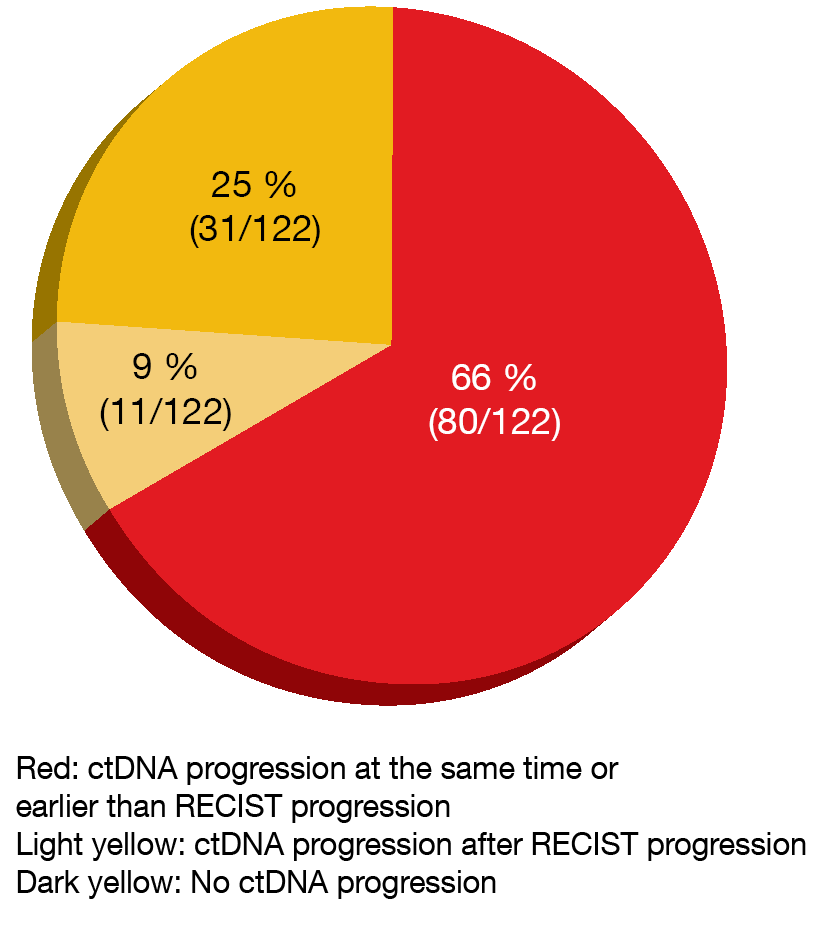
ctDNA progression preceded or co-occurred with disease progression according to RECIST in 66 % of patients across both treatment arms (Figure 2). Median ctDNA progression lead times were similar for osimertinib and comparator EGFR TKI therapy (3.0 vs. 2.6 months). Resistance mutations emerged in 47 % of 122 patients with ctDNA progression. Testing identified C797S mutations in 8 % of the osimertinib-treated population after a median of 16.7 months, while T790M was found in the comparator arm in 74 % after 8.4 months. Overall, the median time from detection of the resistance mutation to RECIST disease progression was 1.4 months. According to this analysis, longitudinal ctDNA monitoring has the potential to detect early signs of progression and acquired resistance mutations ahead of disease progression. Further analyses using next-generation sequencing are ongoing.
Figure 2: Timing of ctDNA progression in relation to the onset of RECIST progression with first-line osimertinib
Insights into osimertinib resistance
Resistance mechanisms to osimertinib treatment were identified by another analysis based on data from 31 patients included in the prospective MATCH-R study [4]. This study assessed the evolution of clonal architecture of tumors from patients treated with targeted drugs. Tissue and plasma biopsies were performed at the time of progression on osimertinib and, optionally, before. All molecular oncogenic alterations were reviewed and classified as definitive/potential resistance mechanisms or concomitant genetic alterations.
This analysis suggested that resistance mechanisms to osimertinib are heterogeneous and more complex than expected. More than one alteration was detected in 45 % of patients; 19 % had one resistance mechanism, 29 % two, and 16 % three. TP53 mutation was the most frequent co-occurring aberration (71 %). Co-occurring genetic alterations correlated significantly with the number of resistance mechanisms (p = 0.002). On-target mechanisms (e. g., EGFR aberrations, RET and MET rearrangements) were identified in 39 %, whereas off-target aberrations (e. g., NTRK1 rearrangements, KIF5B-RET fusions, MET amplifications, KRAS and NRAS mutations) were present in 26 %. In 35 %, the resistance mechanisms remained unknown.
T790M loss co-occurred more frequently with unknown mechanisms of resistance and was associated with a more aggressive progression pattern resulting in shorter time to treatment discontinuation compared to patients who maintained T790M (13 vs. 22 months; HR, 2.16; p = 0.046). Overall, the analysis revealed a considerable number of confirmed fusions (16 %), with some of them being potentially targetable. The scientists stated that combined treatment strategies might be needed to improve clinical outcomes.
GioTag: afatinib followed by osimertinib
Progression on EGFR TKI therapy is inevitable, which raises the question of subsequent treatment. Several considerations provide a rationale for the sequential use of afatinib and osimertinib. The gatekeeper EGFR T790M mutation represents the predominant mechanism of acquired resistance to first- and second-generation EGFR TKIs. T790M incidence rates for the second-generation agent afatinib have been estimated at 50 % to 70 % [5-8] and even 75 % for patients with deletion-19–positive disease [9]. Therefore, most patients progressing on afatinib will be eligible for second-line osimertinib, which has shown pronounced activity against T790M-positive disease in the AURA3 trial [10]. In contrast, no single prevailing resistance mechanism has been identified after progression on osimertinib [11, 12]. Here, targeted options are lacking, and chemotherapy will follow in the majority of cases.
Based on these observations, the global observational GioTag study assessed clinical outcomes in patients who were switched to osimertinib after developing the T790M mutation on first-line treatment with afatinib. Sites in ten countries across Europe, Asia and North America participated in the study. A considerable proportion of patients enrolled in GioTag would have been excluded from clinical trials due to decreased ECOG performance status (PS) or cerebral lesions. ECOG PS ≥ 2 and stable brain metastases were present in 15 % and 10 %, respectively.
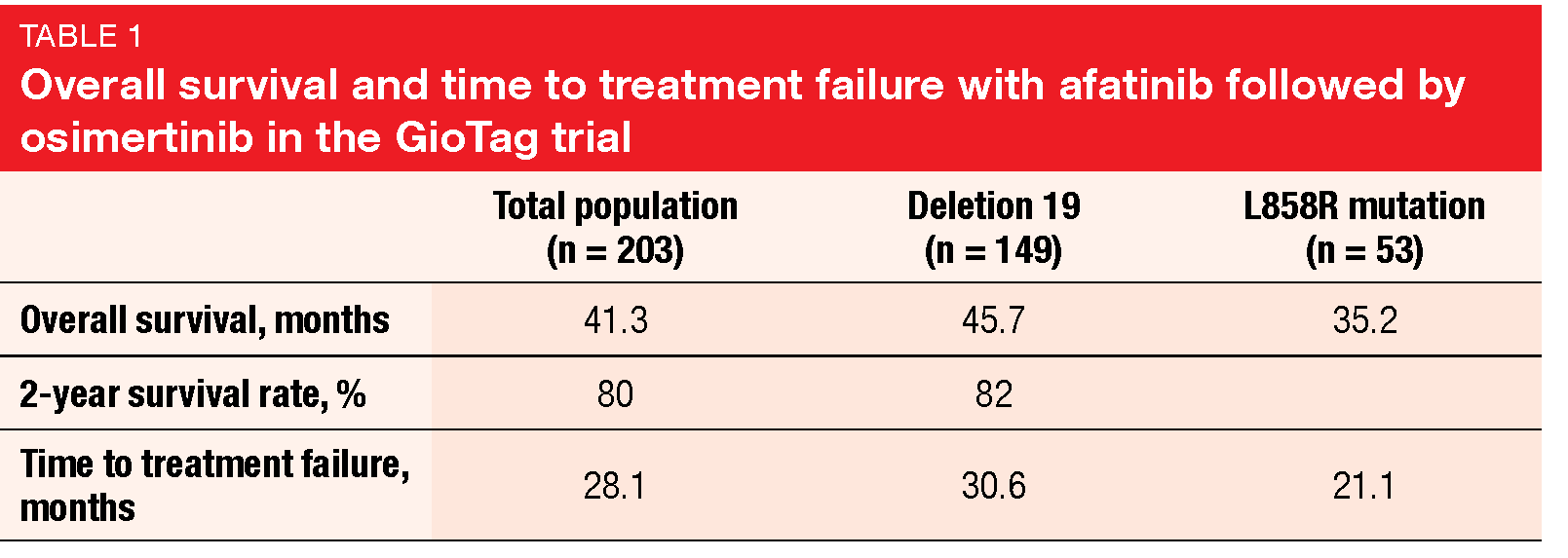
The interim updated analysis reported at ESMO 2019 by Hochmair et al. revealed a median OS of 41.3 months in the total population of 203 patients (Table) [13]. Eighty percent were alive at 24 months. In the group with deletion-19–positive tumors, median OS was 45.7 months, and the 2-year survival rate amounted to 82 %. Median time to treatment failure (TTF) was 28.1 and 30.6 months for the whole group and patients with deletion 19, respectively.
For osimertinib treatment alone, TTF was 15.6 months, which indicates that substantial clinical benefit can be achieved with this agent in the second-line setting following afatinib. In the FLAURA trial, median exposure to first-line osimertinib had been 16.2 months [1]. The authors concluded that sequential afatinib followed by osimertinib is a feasible strategy for patients with EGFR-mutant NSCLC. Prospective data are required to evaluate OS of patients treated with different EGFR TKIs and sequential regimens.
German and French sequencing data
Further real-world analyses add to the evidence supporting sequential treatment. In the prospective, non-interventional real-world GIDEON study that was conducted at 49 centers across Germany, 151 patients with advanced, EGFR-positive NSCLC received frontline afatinib. Data obtained from 29 patients who were treated with afatinib followed by osimertinib in any later line suggest that this regimen might provide optimal outcomes [14]. Two years after the initiation of afatinib treatment, 89.3 % of patients were alive. Median OS data had not reached maturity at the time of the analysis. In keeping with published data [15], the number of patients in the GIDEON study who received later-line osimertinib was higher in the deletion 19 subgroup than in the other EGFR mutation subgroups.
Also, the TKIseq study that was based on the French nationwide claims and hospitalization database identified the sequence as a feasible strategy for patients with acquired T790M mutations [16]. Girard et al. assessed time on treatment, OS, healthcare resources and costs in patients treated with first- or second-generation EGFR TKIs followed by osimertinib in a real-world setting. A total of 576 patients with advanced, EGFR-mutant NSCLC were included in the analysis. Median time on treatment (i.e., duration from the first delivery claim of first- or second-generation TKIs until the discontinuation of osimertinib or death) was 34 months. At 24 months, 64.8 % of patients still received EGFR TKI therapy; at 36 months, this applied to 48.2 %. First-line treatment was administered for a median of 13.6 months, and the median time on osimertinib was 11.9 months. Overall survival for the sequential strategy amounted to 37.1 months. At 36 months, 51.6 % of patients were alive. For the overall population, the mean total direct medical costs per patient per year added up to 62,806 €. The cost of TKI treatment represented 77 % of the overall amount.
First-line afatinib in the real-world setting
Real-world evidence underscores the activity of afatinib as a frontline agent. The global, prospective, single-arm, phase IIIb 1200.55 study evaluated the efficacy and safety of first-line afatinib in a patient population with EGFR-mutated NSCLC [17]. At the time of the analysis, a total of 479 patients had been treated. Most of these had ECOG PS 1 (57 %), and brain metastases were present in 17 %. Thus, the study population contained a certain percentage of patients who would not have been eligible for clinical trials.
Nevertheless, the interim efficacy and safety results were consistent with findings from the pivotal LUX-Lung 3, 6, and 7 trials [18-20]. Median time to symptomatic progression (TTSP) and PFS were 14.9 and 13.4 months, respectively. Clinical benefits occurred across a range of subgroups including patients with ECOG PS 2, asymptomatic brain metastases, uncommon EGFR mutations, and ≥ 1 previous line of therapy. Prolonged efficacy was observed in those with deletion 19 (19.3 and 15.9 months for TTSP and PFS, respectively) and ECOG PS 0/1 (15.8 and 13.8, respectively). Forty-six percent responded to treatment, and 86 % achieved disease control. Diarrhea and rash were the most common adverse events; both were generally manageable with dose reductions and led to few treatment discontinuations (3 % and 1 % for diarrhea and rash, respectively).
A combined analysis pooled the outcomes obtained in the 1200.55 study and another large, prospective phase IIIb trial that evaluated afatinib in EGFR-TKI–naïve patients under real-world conditions [21]. Overall, 1,020 patients were included, 68.8 % of whom had ECOG PS 1. Brain metastases and uncommon EGFR mutations were present at baseline in 18 % each. Thirty-one percent of patients had received one or more previous treatment lines.
This pooled analysis revealed encouraging efficacy as well as a predictable and manageable safety profile consistent with findings from the LUX-Lung trials [18-20]. Median TTSP and PFS in the overall population were 14.6 and 12.9 months, respectively. Objective responses occurred in 52.7 % and lasted for 12.9 months. Almost 90 % of patients achieved disease control, which was maintained for 13.9 months. Dose reductions from 40 mg/d to 30 mg/d were performed in 40.5 %; in another 12.1 %, doses were further reduced to 20 mg/d.
Obstacles to the implementation of sequencing
As the implementation of EGFR TKI sequencing in clinical practice is often difficult, a retrospective analysis conducted in Germany evaluated the clinical course of patients with EGFR-mutant NSCLC who were treated with first-/second-generation TKIs and had their last follow-up after osimertinib approval [22]. The aim of the analysis was to better understand patient disposition and limitations in the real-world setting.
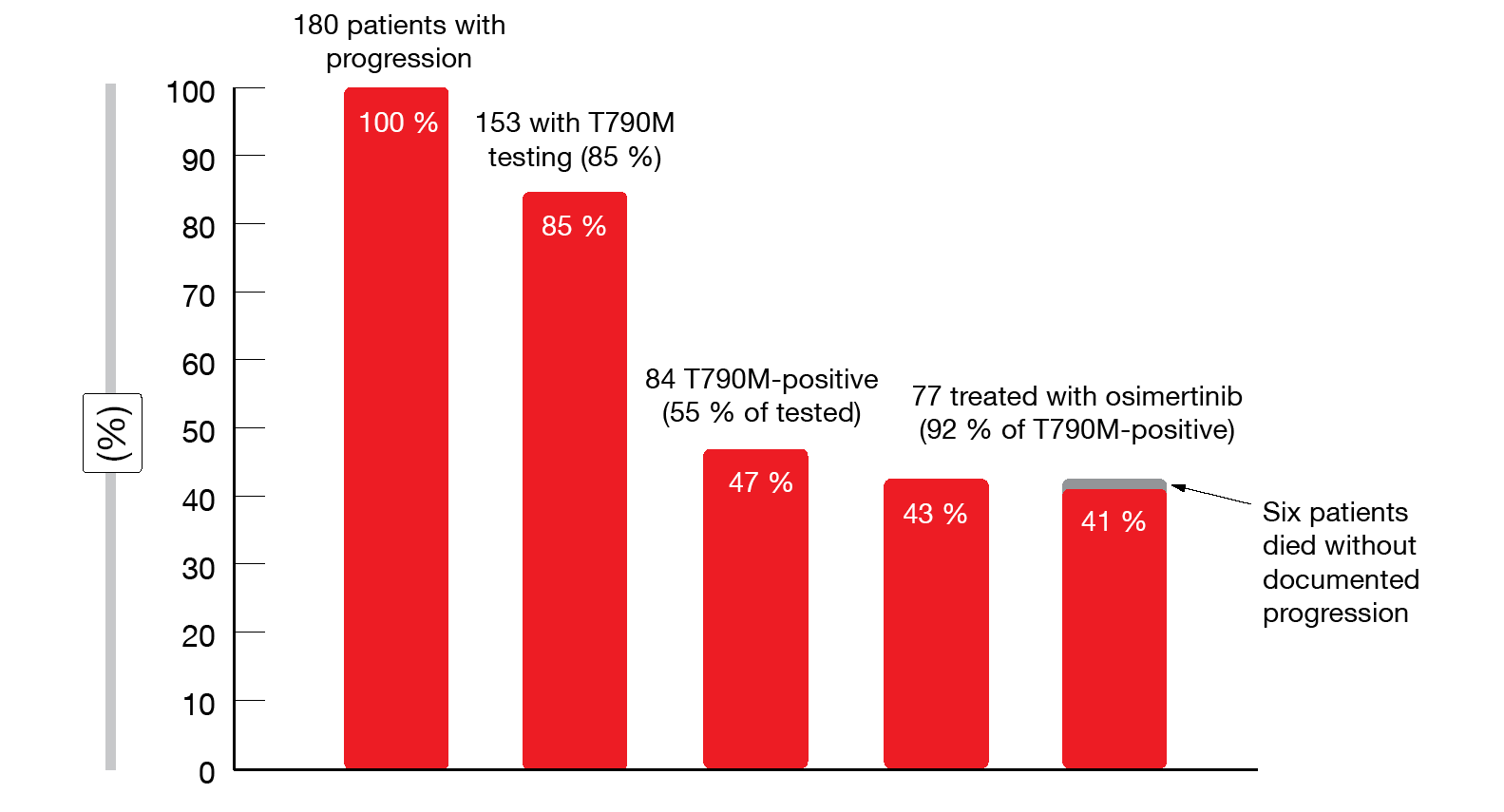
Initial TKI treatment consisted mainly of afatinib (49 %), followed by erlotinib (36 %) and gefitinib (15 %). Within the group of 186 patients with first-/second-generation TKI failure, T790M testing was performed in 153 individuals (85 %), and in 84 (55 %), the T790M mutation was identified (Figure 3). Six patients died without documented progression but had treatment discontinuations or switches mainly due to adverse events. Eventually, 41 % of patients initially treated with first- or second-generation EGFR TKIs received osimertinib. Median OS from the start of the treatment was 35 months for the group with frontline TKI failure. Patients who were prescribed osimertinib thereafter fared significantly better than those with other next-line agents or no subsequent therapy (median OS, 52 vs. 25 months; p < 0.001).
The authors noted that the main obstacles to sequential EGFR TKI treatment were lack of T790M testing and T790M-negative progression. Approximately 25 % of patients did not receive next-line treatment after failure of the first-line EGFR TKI; this percentage was much higher in the group not undergoing T790M testing (77 %) than among T790M-tested patients (14 %). More than 90 % of T790M-positive patients eventually received osimertinib.
Figure 3: T790M testing and osimertinib treatment rate in 186 patients with failure on first- and second-generation EGFR TKI therapy
REFERENCES
- Soria JC et al., Osimertinib in untreated EGFR-mutated advanced non-small-cell lung cancer. N Engl J Med 2018; 378(2): 113-125
- Ramalingam SS et al., Osimertinib vs comparator EGFR-TKI as first-line treatment for EGFRm advanced NSCLC (FLAURA): final overall survival analysis. ESMO 2019, abstract LBA5_PR
- Gray JE et al., Longitudinal circulating tumour DNA (ctDNA) monitoring for early detection of disease progression and resistance in advanced non-small cell lung cancer (NSCLC) in FLAURA. ESMO 2019, abstract LBA85
- Enrico D et al., Multiple synchronous mechanisms may contribute to osimertinib resistance in non-small-cell lung cancer (NSCLC) patients: insights of the MATCH-R study. ESMO 2019, abstract 1526P
- Hochmair MJ et al., Liquid-biopsy-based identification of EGFR T790M mutation-mediated resistance to afatinib treatment in patients with advanced EGFR mutation-positive NSCLC, and subsequent response to osimertinib. Target Oncol 2019; 14(1): 75-83
- Arcila ME et al., Rebiopsy of lung cancer patients with acquired resistance to EGFR inhibitors and enhanced detection of the T790M mutation using a locked nucleic acid-based assay. Clin Cancer Res 2011; 17(5): 1169-1180
- Sequist LV et al., Genotypic and histological evolution of lung cancers acquiring resistance to EGFR inhibitors. Sci Transl Med 2011; 3(75): 75ra26
- Yang JC et al., Osimertinib in pretreated T790M-positive advanced non-small-cell lung cancer: AURA study phase II extension component. J Clin Oncol 2017; 35(12): 1288-1296
- Jenkins S et al., EGFR mutation analysis for prospective patient selection in two phase II registration studies of osimertinib. J Thorac Oncol 2017; 12(8): 1247-1256
- Mok TS et al., Osimertinib or platinum-pemetrexed in EGFR T790M-positive lung cancer. N Engl J Med 2017; 376: 629-640
- Ramalingam SS et al., Mechanisms of acquired resistance to first-line osimertinib: preliminary data from the phase III FLAURA study. Ann Oncol 2018; 29(suppl): LBA50
- Schoenfeld AJ et al., Tissue-based molecular and histological landscape of acquired resistance to osimertinib given initially or at relapse in patients with EGFR-mutant lung cancers. J Clin Oncol 37, 2019 (suppl; abstr 9028)
- Hochmair MJ et al., Afatinib followed by osimertinib in patients with EGFR mutation-positive advanced NSCLC: updated data from the GioTag real-world study. ESMO 2019, abstract 1532P
- Brückl W et al., Sequential treatment with afatinib followed by 3rd generation EGFR-TKI: subgroup analysis of the GIDEON trial – a prospective non-interventional study in EGFR-mutated NSCLC patients in Germany. ESMO 2019, abstract 1527P
- Mok T et al., Osimertinib or platinum-pemetrexed in EGFR T790M-positive lung cancer. N Engl J Med 2017; 376: 629-640
- Girard N et al., TKIseq study: efficacy and burden of TKI sequence of first and second generation followed by osimertinib in non-small-cell lung cancer in the French real-world setting. ESMO 2019, abstract 1528P
- De Marinis F et al., Afatinib in EGFR TKI-naïve patients with EGFR mutation-positive NSCLC: interim analysis of a phase IIIb, multi-national, open-label study. ESMO 2019, abstract 1472P
- Sequist LV et al., Phase III study of afatinib or cisplatin plus pemetrexed in patients with metastatic lung adenocarcinoma with EGFR mutations. J Clin Oncol 2013; 31: 3327-3334
- Wu Y-L et al., Afatinib versus cisplatin plus gemcitabine for first-line treatment of Asian patients with advanced non-small-cell lung cancer harbouring EGFR mutations (LUX-Lung 6): an open-label, randomised phase 3 trial. Lancet Oncol 2014; 15: 213-222
- Park K et al., Afatinib versus gefitinib as first-line treatment of patients with EGFR mutation-positive non-small-cell lung cancer (LUX-Lung 7): a phase 2B, open-label, randomised controlled trial. Lancet Oncol 2016; 17: 577-589
- De Marinis F et al., A combined analysis of two phase IIIb studies of afatinib in EGFR TKI-naïve patients with EGFR mutation-positive NSCLC. ESMO 2019, abstract 1474P
- Christopoulos P et al., Real-world implementation of sequential targeted therapies for EGFR-mutated NSCLC. ESMO 2019, abstract 1538P