How to approach translational research as a clinician
A career as a physician scientist can be extremely fulfilling, as it is an opportunity to make a difference in patient care by way of academic excellence. Clinical observations are explored in the translational setting based on experience and prior knowledge; eventually, the insights gained in this way can give rise to clinical innovation. For instance, a translational program is built around patients progressing on a particular targeted treatment, and new resistance mutations are identified based the analysis of repeated biopsies.
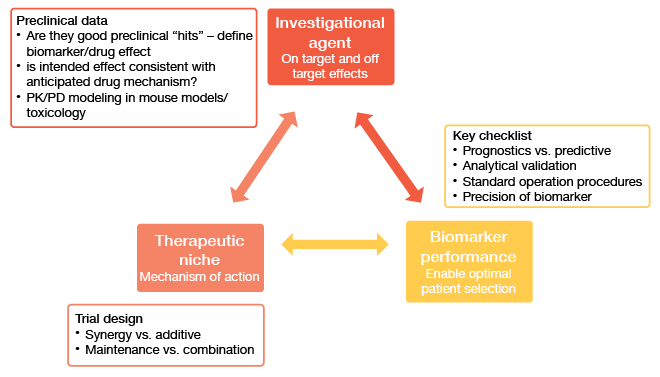
The drug development paradigms are constantly evolving. In the setting of targeted treatment, critical evaluation of the therapeutic effects of an investigational agent includes on-target and off-target effects, the therapeutic niche, and biomarker performance (Figure 1). Against the background of the enormous biological heterogeneity of cancer cells, there is no lack of issues worth assessing. If possible, issues should be explored that no one else is working on.
Figure 1: Critical evaluation of the therapeutic effect of a drug
The pivotal roles of mentorship and the team
Young researchers benefit from mentors who open doors for grants or publications and provide opportunities to learn and grow. Ideally, mentorship creates a safe environment and facilitates autonomy as well as scientific independence. The mentor does not necessarily have to work at the researcher’s institution.
Also, team collaboration is indispensable. It is important to find like-minded research partners. Challenging tasks such as the identification of a high-precision biomarker require dividing the research program into layers that are dealt with by different teams. For example, the Singapore-based Translational and Clinical Research Flagship Programme consists of three teams that are assessing cancer stem cell biology, genomics, and translational therapeutics. It was demonstrated that the number and distribution of driver aberrations in EGFR-mutant NSCLC shows great variety, which is also true for the same patient over time [1]. Co-drivers, which especially accumulate in smokers, can portend poor outcomes. According to these insights, the genomic landscape dictates clinical trajectories.
Learning from exceptional responders
Even negative trials can provide precious clues. In a study investigating gefitinib plus radiochemotherapy, two exceptional responders showed a silent mutation, which was a single nucleotide polymorphism Q787Q [2]. Other non-canonical mechanisms of EGFR addiction were therefore assessed in patient-derived cell lines. This analysis revealed that EGFR TKI sensitivity varies considerably according to Q787Q genotype [3]. The key experiment to prove this observation was single nucleotide editing, which indeed induced TKI sensitivity. Long non-coding RNA EGFR-AS1 that mediates EGFR addiction turned out to be sufficient to cause resistance. This new EGFR-mediated mechanism could be explored in the future.
Developing a strategy for a research career
The “research startup” calls for some basic traits, such as curiosity, creativity, and conviction. Formal education is always useful. Moreover, the research track entails the acquisition of experience in translational research, manuscripts, and grants. Young researchers should not be picky but rather take any chance to publish a paper, even if it is for a less renowned journal. There is a need to differentiate between performing research on a professional level and on a hobbyist level; the former takes more time and requires continuous training, deep knowledge, high discipline and lifelong learning.
With regard to developing a scientific framework for clinical practice, the significance of relationships must not be underestimated. Managing relationships is crucial; this applies to the clinical team as well as to patients, departments, mentors, trial coordinators, scientific collaborators, journal editors, industry representatives and national/ regional program representatives. International connections allow for being part of a broader community, e.g. JSMO or the International Association for the Study of Lung Cancer (IASLC). The “ripple” effect of research excellence includes the impact on clinical service, opportunities for mentorship and enhanced relationships with colleagues.
Challenges for the clinician-scientist
The worlds of clinicians and scientists differ in fundamental ways. Clinicians think in a parallel manner and receive immediate gratification when the patient responds, although they are operating in uncertainty. On the other hand, scientists think sequentially, experience delayed gratification and engage in controlled experiments. There are synergies and common traits as well, but it is up to the individual to decide which part of the spectrum they find more appealing. Young physicians needs to be aware of their traits, interests and motivations.
Perspective is important, as getting tunnel-visioned should be avoided. Generally, the clinical-scientist should not be overly focused on his or her work; it is necessary to take time off and to pursue hobbies and sports.
Overall, it is commendable to play to one’s strengths and take some calculated risks, as there will be some uncertainty one operates under. Persistence and luck are necessary ingredients for the physician scientist’s career. By setting up conditions that allow for good opportunities, it is possible to capitalize in the best possible way when luck comes round.
REFERENCES
- Nahar et al., in press, Nature Communications
- Tan EH et al., Gefitinib, cisplatin, and concurrent radiotherapy for locally advanced head and neck cancer: EGFR FISH, protein expression, and mutational status are not predictive biomarkers. Ann Oncol 2012; 23(4): 1010-1016
- Tan DSW et al., Long noncoding RNA EGFR-AS1 mediates epidermal growth factor receptor addiction and modulates treatment response in squamous cell carcinoma. Nat Med 2017; 23(10): 1167-1175