Waldenström’s macroglobulinemia: BTK inhibition and other treatments
Within the group of non-Hodgkin lymphoma, Waldenström’s macroglobulinemia (WM), an indolent B-cell lymphoplasmacytic lymphoma, accounts for approximately 2 % of cases [1]. This disease is deemed incurable and typically involves infiltration of tissues such as bone marrow, lymph nodes and/or spleen with clonal lymphoplasmacytic cells, as well as serum monoclonal paraprotein production. The B-cell receptor signaling pathway is constitutively activated in WM [2, 3]. In more than 90 % of patients, MYD88 mutations can be found.
As Bruton’s tyrosine kinase (BTK) represents an integral component of the B-cell receptor signaling pathway, BTK inhibition has emerged as a new treatment standard. BTK inhibitors that are currently in use or are being clinically evaluated include the first-generation agent ibrutinib that has been licensed for the treatment of WM in the USA and the EU, and second-generation agents with improved efficacy and tolerability.
ASPEN: zanubrutinib vs. ibrutinib
The selective, irreversible second-generation BTK inhibitor zanubrutinib has been designed to maximize BTK occupancy and to minimize off-target inhibition of other kinases [4]. Zanubrutinib is as potent against BTK as ibrutinib, but its increased selectivity allows for an optimized adverse event (AE) profile [4, 5]. Its efficacy and safety in WM are being assessed in the ongoing open-label, multicenter, randomized phase III ASPEN study. At EHA 2020, Dimopoulos et al. reported the results for Cohort 1, which included patients with MYD88-mutated WM who met at least one criterion for treatment initiation and had not received prior BTK inhibition [6]. They were treated with either zanubrutinib 160 mg twice daily (BID; n = 102) or ibrutinib 420 mg daily (n = 99). Both pretreated and treatment-naïve patients participated; enrollment of the latter was only permitted if they were considered unsuitable for standard chemoimmunotherapy. Out of 201 individuals, 164 had relapsed or refractory disease.
Superiority of zanubrutinib versus ibrutinib with respect to the rate of complete responses (CRs) plus very good partial responses (VGPRs) in the relapsed/refractory group according to independent review was defined as the primary endpoint. Although this analysis only revealed a trend in favor of zanubrutinib (28.4 % vs. 19.2 %; p = 0.0921), superior efficacy of the second-generation agent with respect to CR plus VGPR was demonstrated according to investigator assessment (secondary endpoint; 30.4 % vs. 18.2 %; p = 0.0302; Figure 1). Major responses emerged in approximately 78 % in both arms. Also, with regard to IgM levels, zanubrutinib induced a significantly deeper reduction over time (p = 0.037). Both arms showed excellent event-free rates at 12 months for progression-free survival (PFS; 89.7 % vs. 87.2 %) and overall survival (OS; 97.0 % vs 93.9 %).
Figure 1: ASPEN trial: Response rates observed with ibrutinib vs. zanubrutinib according to the investigators
Lower incidence of adverse events
Zanubrutinib demonstrated clinically meaningful advantages in terms of safety and tolerability. AEs leading to death or treatment interruption and discontinuation emerged less frequently in the experimental arm. The risk of atrial fibrillation or flutter was significantly reduced (2.0 % vs. 15.3 %), as were the rates for diarrhea (20.8 % vs. 31.6 %), major hemorrhage (5.9 % vs. 9.2 %), and hypertension (10.9 % vs. 17.3 %). While the incidence of atrial fibrillation/flutter increased constantly over time in ibrutinib-treated patients, it remained stable at a low level in the zanubrutinib-treated group. A similar trajectory became evident for hypertension. Infections did not occur more frequently in the experimental arm (66. 3 % vs. 67.3 %) despite higher rates of neutropenia (29.7 % vs. 13.3 %). Quality-of-life analyses demonstrated improvement for both drugs over time, although the zanubrutinib-treated patients who achieved VGPR showed a more favorable course that probably reflects improved safety and tolerability.
The results for Cohort 1 of the ASPEN study have already been presented at the 2020 ASCO Virtual Meeting [7] and were included in the ASCO highlight session on hematologic malignancies. In her discussion of the findings, Nancy Bartlett, MD, Washington University, St. Louis, USA, pointed out that longer follow-up might be necessary for obtaining deeper responses. Given the higher tolerability of the new-generation BTK inhibitor, Dr. Bartlett noted that in her opinion, zanubrutinib will be the therapy of choice once it has received approval for the treatment of patients with WM.
Assessment in WM patients with MYD88 wildtype
In Cohort 2 of the ASPEN study, zanubrutinib 160 mg BID was assessed in treatment-naïve and pretreated WM patients who had MYD88 wildtype [8] based on the observation that response rates and survival are worse with ibrutinib in the absence of MYD88 mutations [9-11]. Twenty-eight patients were enrolled 26 of whom had MYD88 wildtype, while the mutation status was unknown in two. Relapsed or refractory disease was present in 23 individuals. After a median follow-up of 17.9 months, 17 (60.7 %) were still on study treatment.
Single-agent zanubrutinib resulted in a major response rate of 50.0 %, including VGPR in 26.9 %. Patients with relapsed/refractory disease had a higher major response rate than the treatment-naïve group (52.4 % and 40.0 %, respectively). The median time to first major response was 2.9 months. One patient obtained IgM CR. Median PFS and OS had not been reached yet; event-free rates at 12 months were 72.4 % and 96.2 %, respectively. Zanubrutinib was well tolerated, with disease progression representing the primary reason for treatment discontinuation. The AE profile was consistent with that observed in Cohort 1. No fatal AEs were reported. At 3.6 %, the rate of all-grade atrial fibrillation/flutter was low.
Three-year update of phase I/II results
Opat et al. reported the three-year update of the first-in-human, multicenter, phase I/II AU-003 study that was designed to evaluate the safety, pharmacokinetics and anti-tumor activity of single-agent zanubrutinib in patients with B-cell malignancies [12]. Seventy-seven patients with WM were treated in this trial. Among these, 24 had been treatment-naïve prior to study inclusion, while 53 had relapsed/refractory disease.
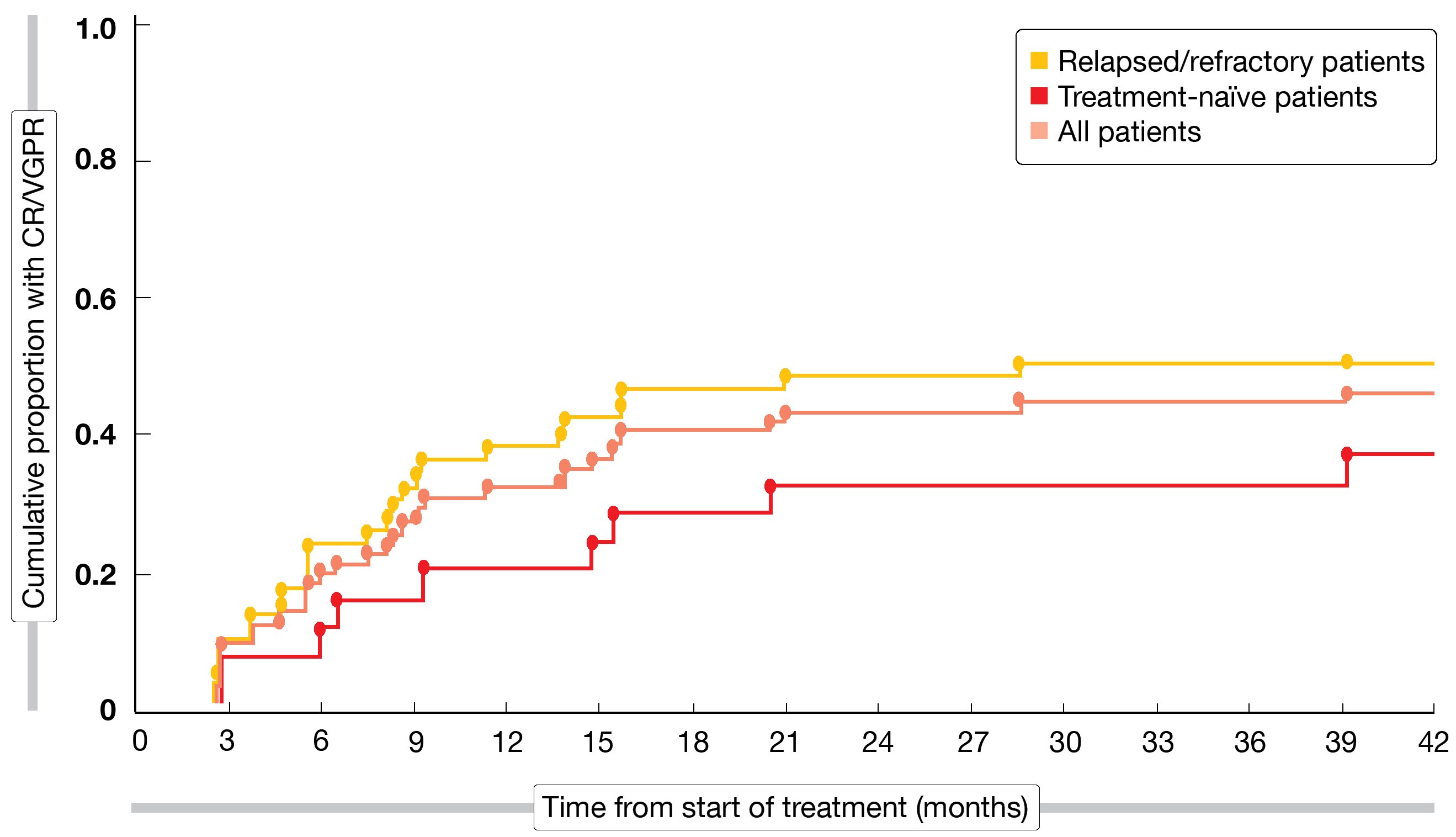
After a follow-up of 35.3 months, deep responses were observed in both treatment-naïve and relapsed/refractory settings and in all molecular subtypes including MYD88 wildtype. The overall response rate (ORR) was 96 % in the total evaluable group (n = 73), with an excellent CR/VGPR rate of 46 %. Kaplan-Meier estimates of the cumulative proportion of patients with CR/VGPR showed that the rate increased over time (Figure 2). At 36 months, 80.3 % and 83.4 % of patients were progression-free and alive, respectively. Median hemoglobin and IgM levels showed fast improvement after the initiation of treatment and remained stable over time.
Long-term treatment with zanubrutinib was generally well tolerated. AEs led to treatment discontinuation in 13.0 %. Among AEs of interest, infections occurred most frequently, followed by bruising and minor bleeding. Grade ≥ 3 infections were most common in the first year of treatment and decreased thereafter, while the percentage of patients affected by hypertension increased over time. The rate of grade ≥ 3 atrial fibrillation/flutter was 1.3 %.
Figure 2: Increases in the rates of patients with CR and VGPR over time with zanubrutinib
Ixazomib plus rituximab and dexamethasone
The combined regimen of the proteasome inhibitor ixazomib, the anti-CD20 antibody rituximab and dexamethasone (IRd) showed favorable clinical activity in the relapsed/refractory setting according to the recent analysis of the prospective, international, phase I/II HOVON124/ECWM-R2 study [13]. Phase I of this trial identified ixazomib 4 mg on days 1, 8 and 15 every 28 days as the recommended phase II dose. Rituximab 1,400 mg was administered on day 1 of cycles 3 to 8, and dexamethasone 20 mg on days 1, 8, 15 and 22 of each cycle. The induction therapy consisted of 8 cycles. Responders who achieved at least stable disease went on to receive maintenance with rituximab 1,400 mg every 3 months for 2 years. ORR after induction based on the IgM levels was defined as the primary outcome. Forty-five patients completed all eight cycles, and 41 continued on to maintenance.
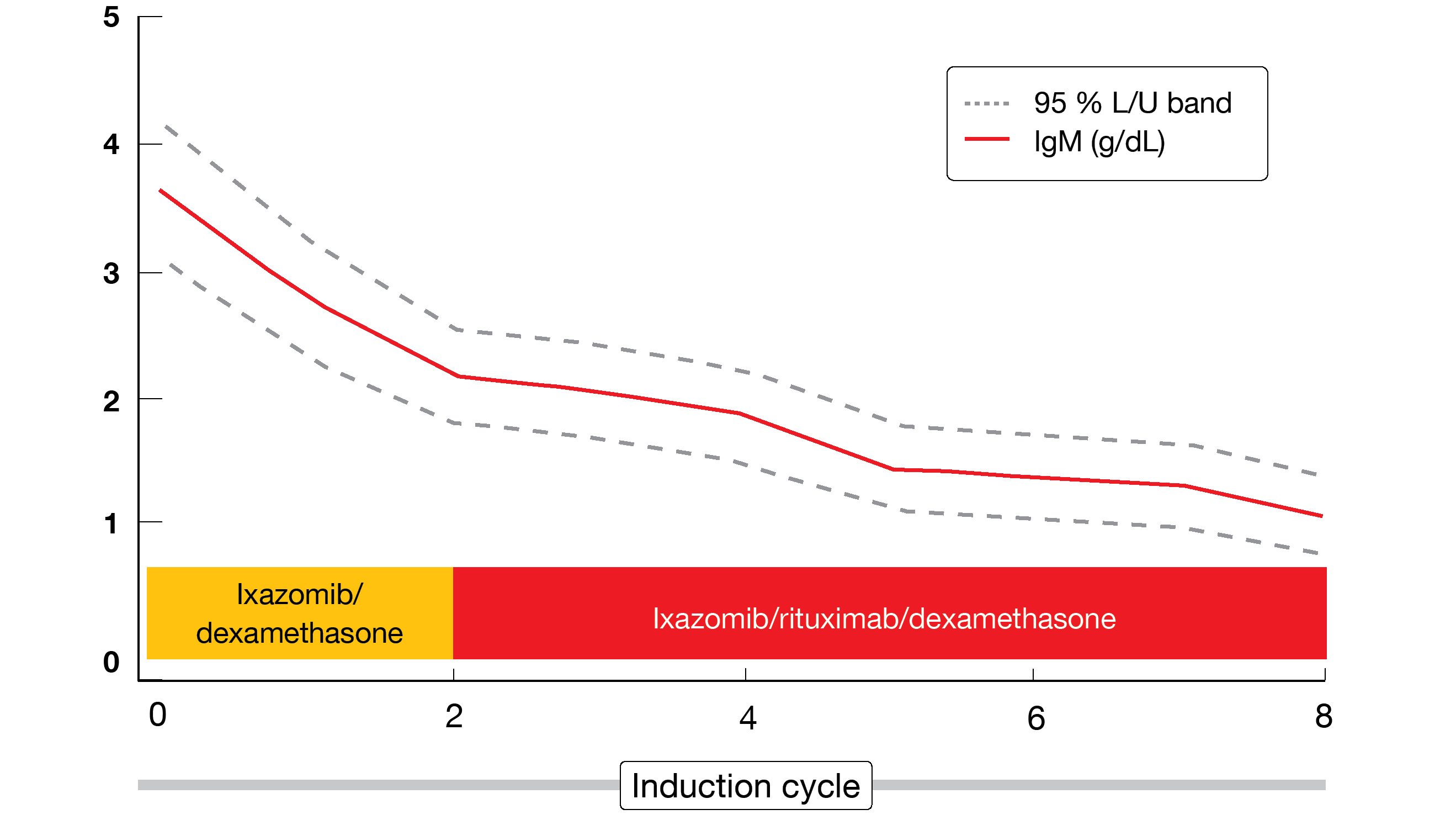
IRd was shown to be a feasible and active regimen with high ease of administration. The primary endpoint was met, with an ORR of 71 %; 51 % of patients achieved at least partial remissions. With regard to best response obtained during the induction phase, the ORR was 85 %. Significant IgM and hemoglobin responses already occurred before the start of rituximab treatment. The IgM levels decreased between baseline and cycle 2 (p < 0.0001; Figure 3), while the hemoglobin levels simultaneously increased (p = 0.0004). IgM flares were not observed. Median PFS, OS and duration of response had not been reached at the time of the analysis. At 24 months, 56 % of patients were progression-free and 88 % were alive.
Although neuropathy worsened or emerged in 16 patients, it was mostly grade 1 or 2 and reversible in 10 individuals. Patient-reported outcomes according to the EORTC QLQ-CIPN20 questionnaire demonstrated that the neuropathy-associated symptom burden did not increase during treatment. The majority of AEs were grades 1 and 2; no grade-4 AEs occurred. Global health status improved significantly during induction according to the EORTC HR-QoL QLQ-C30 questionnaire (p = 0.03 in cycle 8 vs. baseline).
Figure 3: IgM response with ixazomib/rituximab/dexamethasone: decrease in IgM levels even prior to the initiation of rituximab treatment
Bendamustine and rituximab
International consensus guidelines recommend the combination of bendamustine and rituximab for the treatment of WM in both frontline and relapsed settings [14]. However, the optimal dose and schedule of this regimen has not been well established yet. An international, multicenter, retrospective cohort analysis assessed clinical outcomes in untreated or relapsed consecutive WM patients who received bendamustine with or without rituximab [15]. Overall, 217 individuals were included in the analysis; among these, 122 had been treated in the frontline setting.
The outcomes obtained in this unselected group were excellent, with more favorable results in hitherto untreated patients. These tolerated higher total doses of bendamustine than relapsed patients and achieved comparatively deeper responses with higher combined rates of CR and VGPR (47.5 % vs. 20 %; p < 0.001). PFS was significantly longer in the frontline setting (p < 0.05) and also varied according to the depth of response, with 2-year PFS rates of 98.2 % vs. 84.3 % for patients achieving CR/VGPR vs. PR (p < 0.001). Performance status and total bendamustine dose affected both depth of response and PFS. A total bendamustine dose of ≥ 800 mg/m2 was shown to be critical for obtaining a depth of response sufficient to achieve durable remissions. Surrogate markers of toxicity including truncation of treatment were less frequent in the frontline setting.
REFERENCES
- Swerdlow SH et al., Lymphoplasmacytic lymphoma. In: WHO Classification of Tumours of Hematopoietic and Lymphoid Tissues, revised 4th Edition. 232-235 IARC, Lyon, 2017
- Rickert RC, New insights into pre-BCR and BCR signalling with relevance to B cell malignancies. Nat Rev Immunol 2013; 13(8): 578-591
- Argyropoulos KV et al., Clonal B cells in Waldenström’s macroglobulinemia exhibit functional features of chronic active B-cell receptor signaling. Leukemia 2016; 30(5): 1116-1125
- Guo Y et al., Discovery of zanubrutinib (BGB-3111), a novel, potent, and selective covalent inhibitor of bruton’s tyrosine kinase; J Med Chem 2019; 62(17): 7923-7940
- Tam CS et al., Phase 1 study of the selective BTK inhibitor zanubrutinib in B-cell malignancies and safety and efficacy evaluation in CLL. Blood 2019; 134(11): 851-859
- Dimopoulos M et al., ASPEN: Results of phase 3 randomized trial of zanubrutinib versus ibrutinib for patients with Waldenström macroglobulinemia. EHA 2020, abstract S225
- Tam C et al., ASPEN: Results of a phase III randomized trial of zanubrutinib versus ibrutinib for patients with Waldenström macroglobulinemia (WM). J Clin Oncol 38: 2020 (suppl; abstr 8007
- Dimopoulos M et al., Updated results of the ASPEN trial from a cohort of patients with MYD88 wild-type Waldenström macroglobulinemia. EHA 2020, abstract EP1180
- Treon SP et al., Ibrutinib in previously treated Waldenström’s macroglobulinemia. N Engl J Med 2015; 372(15): 1430-1440
- Treon SP et al., MYD88 mutations and response to ibrutinib in Waldenström’s macroglobulinemia. N Engl J Med 2015; 373(6): 584-586
- Treon SP et al., MYD88 and CXCR4 mutation status as determinants of ibrutinib activity in Waldenström’s Macroglobulinemia. IWWM-9 Session, 9 October 7, 2016
- Opat S et al., Zanubrutinib for the treatment of patients with Waldenström macroglobulinemia: Three years of follow-up. EHA 2020, abstract EP1168
- Kersten MJ et al., Ixazomib, rituximab and dexamethasone in patients with relapsed or progressive Waldenström’s macroglobulinemia: Final analysis of the HOVON124/ECWM-R2 trial. EHA 2020, abstract S226
- Leblond V et al., Treatment recommendations from the Eighth International Workshop on Waldenström’s macroglobulinemia. Blood 2016; 128(10): 1321-1328
- Arulogun S et al., Bendamustine plus rituximab in Waldenström macroglobulinaemia: deeper responses, longer survival and less toxicity in the frontline setting. EHA 2020, abstract 1194