Expanding treatment options in NSCLC patients with rare mutations: ALK, ROS1, MET, BRAF
ALK gene rearrangements occur in approximately 4 %to 5 % of all Caucasian and Asian patients with advanced NSCLC. Crizotinib was the first approved ALK inhibitor and is the current front-line standard treatment for ALK-positive NSCLC. However, despite initial responses to TKI treatment, all of these patients relapse in the long run. This is mainly due to secondary mutations in the ALK or ROS1 kinase domains, or poor CNS drug penetration. Secondary mutations have been observed in approximately 25 % of patients with resistance to crizotinib [1, 2]. Research is focussing on the development of new options for both first-line and resistant settings.
The J-ALEX frontline trial: alectinib versus crizotinib
Alectinib is a potent, highly selective, CNS-active ALK inhibitor with activity against ALK-resistance mutations. The J-ALEX phase III study compared alectinib 300 mg BID (n = 103) with crizotinib 250 mg BID (n = 104) in ALK-inhibitor- naïve patients with stage IIIB/IV or recurrent ALK-positive NSCLC [3]. Patients with treated or asymptomatic brain metastases were eligible.
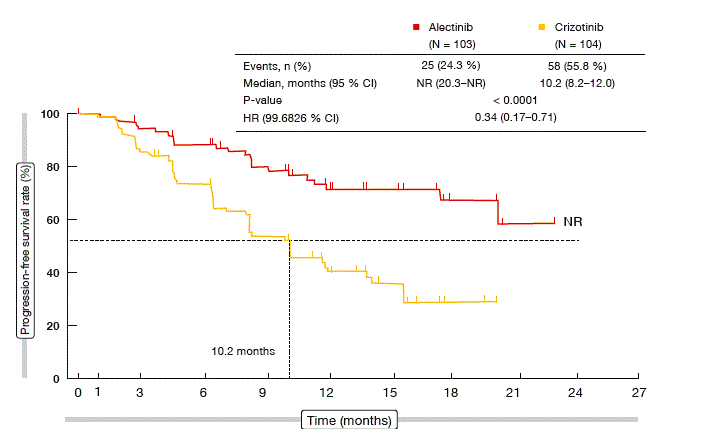
J-ALEX has already met the primary endpoint, which was PFS, at a preplanned interim analysis, as assessed by an independent review facility. These findings suggested a highly significant difference in favour of alectinib (median PFS, not reached vs. 10.2 months; HR, 0.34; p > 0.0001; Figure). Almost all of the patients derived a PFS benefit from the alectinib treatment, according to a subgroup analysis. ORRs assessed through the independent review facility were 91.6 % and 78.9 % for alectinib and crizotinib, respectively. The waterfall plots indicated greater tumour shrinkage in the alectinib arm.
Figure: J-ALEX-study: superiority of alectinib over crizotinib with regard to PFS (ITT population)
Alectinib was well tolerated, and showed a favourable AE profile. Patients in both arms reported constipation, nasopharyngitis, dysgeusia, nausea, pyrexia, diarrhoea and vomiting. All of these AEs occurred less frequently with alectinib than with crizotinib, and sometimes by a very large margin. This was also true for elevation of the liver enzymes. Grade 3/4 AE rates were halved with alectinib compared to crizotinib (26.2 % vs. 51.9 %), and the AEs necessitated both discontinuations and dose interruptions to markedly lower levels in the experimental arm than the control arm. Overall, these results suggest that alectinib has the potential to be a new first-line standard for patients with ALK-positive NSCLC.
Brigantinib in crizotinib-refractory patients: ALTA
Brigantinib is an investigational next-generation ALK TKI, which was designed to have potent and broad activity against resistant ALK mutations. Phase II data presented at the ASCO Congress demonstrated activity of this agent after progression on crizotinib. The international, randomised, dose-evaluation ALTA trial evaluated brigantinib in patients with locally advanced or metastatic ALK-positive NSCLC [4]. The patients received brigantinib at two doses in a randomised manner: 180 mg OD (n = 110), which was preceded by a 7-day lead-in at 90 mg, or 90 mg OD (n = 112). The primary endpoint was ORR according to the RECIST criteria.
Patients in the 180 mg and 90 mg brigantinib groups achieved confirmed ORRs of 54 % and 45 %, respectively. The majority experienced PR. Confirmed CRs occurred in 4 and 1 patients, respectively. ORRs did not differ by history of chemotherapy. Most of the patients in both groups showed reductions in tumour size. Disease control was achieved in 86 % and 82 %, respectively. Median PFS exceeded 1 year in the 180 mg dose group (12.9 months), while it was only 9.2 months in the 90 mg dose group. At 1 year, 54 % and 39 % of patients were alive and progression free, respectively. Median OS had not yet been reached in either group. The proportions of patients alive at 1 year were 80 % and 71 %, respectively.
Activity against brain lesions
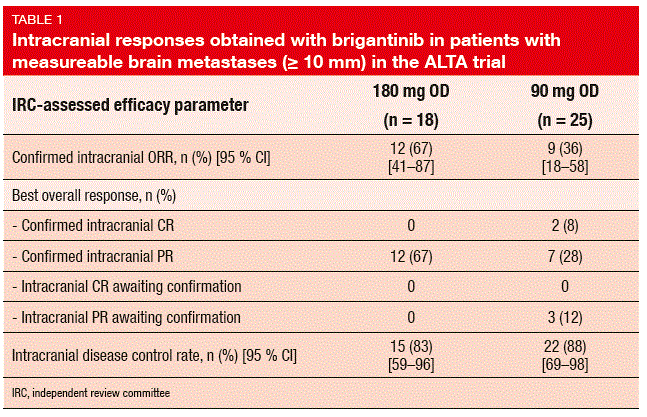
Intracranial responses occurred in both dose groups, as assessed by an independent review committee. In patients with measurable (≥ 10 mm) lesions, the confirmed intracranial ORRs were 67 % versus 36 % with the 180 mg and 90 mg doses, respectively. Intracranial disease control occurred in 83 % and 88 %, respectively (Table 1). Patients with measurable, active brain metastases (with no prior radiotherapy, or progression after radiotherapy) at baseline attained intracranial ORRs of 73 % and 37 %, respectively. Intracranial PFS had not been reached with the 180 mg treatment, and was 15.6 months with the 90 mg schedule.
Brigantinib demonstrated an acceptable safety profile in both arms. Nausea, diarrhoea, headache, cough and fatigue were reported most frequently. Grade 3/4 AE rates were low. The authors concluded that brigantinib has the potential to be a new treatment option for patients with crizotinib-resistant ALK-positive NSCLC. The efficacy and safety findings support the choice of the 180-mg regimen for further trials. A randomised phase III study is currently comparing brigantinib 180 mg with crizotinib in ALK-inhibitor-naïve patients.
Novel ALK- and ROS1-inhibiting compound: lorlatinib
Lorlatinib is a novel macrocyclic ALK inhibitor that is able to penetrate into the CNS. It has shown activity against a wide range of mutations that confer resistance to ALK inhibitors, and it is also a potent inhibitor of ROS1.
Solomon et al. presented the dose escalation component of an ongoing phase I/II study evaluating lorlatinib OD or BID in 54 patients with advanced, ALK/ROS1-positive NSCLC [5]. These patients were either treatment-naïve or had experienced disease progression after at least one prior ALK/ROS1 TKI. Any prior chemotherapy was allowed. Measureable extracranial disease had to be present. Asymptomatic CNS metastases (treated or untreated) were allowed; 72 % of the patients had brain metastases. The intracranial activity of lorlatinib was prospectively assessed using MRI.
Lorlatinib showed robust clinical activity in both ALK-positive and ROS1-positive patients. This treatment gave rise to three CRs and 16 PRs, resulting in an ORR of 46 %. Patients who had received one prior ALK TKI showed an ORR of 57 %, while those after at least two ALK TKIs achieved an ORR of 42 %. The majority developed decreases in target lesion size. In 20 patients, the responses were ongoing at the time of the data cut-off. Median PFS was 11.4 months for the entire cohort. At one year, 41 % were free of progression. As for ORR, the group that had previously received only one ALK TKI fared better with regard to PFS than those who had been treated with two or more TKIs (PFS, 13.5 vs. 9.2 months).
Lorlatinib treatment prompted significant intracranial responses. According to the prospective intracranial assessment, five CRs and two confirmed PRs occurred in 18 patients with measurable intracranial disease, which amounted to a confirmed intracranial response rate of 39 %. Three of four ROS1-positive patients with measureable intracranial disease experienced tumour reductions. Responses also occurred in patients with leptomeningeal disease.
Hypercholesterolaemia was the most frequent treatment-related AE, but it was asymptomatic and readily managed with statin therapy. At the recommended phase II dose of 100 mg OD, other AEs were seen, included peripheral oedema, hypertriglyceridaemia, and slowing of speech. The phase II portion of this study is ongoing in 57 centres worldwide.
Crizotinib in NSCLC with MET alterations
Mutations in the known proto-oncogene MET that lead to decreased MET degradation occur in approximately 3 % to 4 % of patients with non-squamous NSCLC. MET exon 14 alterations represent a heterogeneous group of mutations. While many of these result in MET exon 14 skipping, select point mutations or deletions create the same biology without causing exon skipping. Concurrent MET amplification can be identified in 15 % to 20 % of cases.
Crizotinib was initially developed as a MET inhibitor, and it is currently being tested in patients with advanced MET exon-14-altered NSCLC in the open-label, multi-centre, phase I PROFILE 1001 study. Results presented at the ASCO Congress showed that in these patients, crizotinib has anti-tumour activity and a generally tolerable AE profile, which is consistent with that previously reported for patients with ALK-positive or ROS1– rearranged NSCLC [6].
Twenty-one patients were enrolled and received crizotinib at a starting dose of 250 mg BID. None of their tumours harboured concurrent ALK or ROS1 aberrations. Crizotinib therapy prompted an ORR of 44 % in the PROFILE 1001 trial. Almost all of the patients achieved disease shrinkage. Responses were usually observed early on, and most patients remained on study, with the longest ongoing response of approximately 1 year. Median PFS and OS could not be calculated, as no deaths or disease progressions had occurred at the time of the data cut-off.
The predominant treatment-related AEs were oedema, nausea, diarrhoea, and vision disorder, with the majority of these being rated as grade 1 or 2. According to the trial authors, further study of crizotinib in this patient population is warranted.
BRAF mutation as a target
BRAF V600E mutations occur in 1 % to 2 % of patients with adenocarcinoma of the lung. Among these mutations, 70 % are of the BRAF V600E type. NSCLC that shows BRAF V600E mutation has histological features that are suggestive of an aggressive tumour, and patients demonstrate less favourable outcomes when treated with platinum-based chemotherapy.
An efficient targeted approach in this group includes the BRAF-inhibiting small molecule dabrafenib in combination with the small molecule trametinib, which acts as an allosteric inhibitor of MEK1 and MEK2. Together, these drugs confer dual inhibition of the MAPK pathway. In the multi-cohort, non-randomised, open-label phase II BRF113928 study, which involved 78 patients with BRAF V600E-mutated stage IV NSCLC, dabrafenib monotherapy yielded an ORR of 33 % and a median PFS of 5.5 months after failure of ≥ 1 prior platinum-based therapy for advanced disease (Cohort A) [7]. At the ASCO Congress, Planchard et al. presented their primary analysis of Cohort B of this trial; these patients were treated with the combination of dabrafenib 150 mg BID and trametinib 2 mg OD after at least one platinum-based chemotherapy and not more than three previous lines of treatment [8]. The primary objective was investigator-assessed ORR.
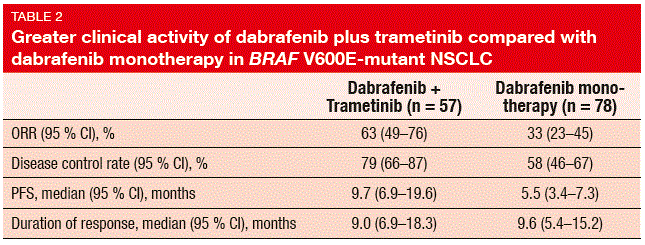
Fifty-seven patients were evaluable for response, all of whom had non-squamous histology. In this group, ORR was 63 %, with a disease control rate of 79 %. Responses lasted for a median interval of 9.0 months, and half of the confirmed responses were ongoing at the time of analysis. For median PFS, the analysis yielded 9.7 months. As compared to dabrafenib monotherapy (Cohort A of the BRF113928 study), dabrafenib plus trametinib showed greater clinical activity (Table 2).
The AE profile was manageable and similar to previous observations obtained with the treatment of melanoma patients. AEs included pyrexia, nausea, vomiting, diarrhoea, asthenia, decreased appetite, chills, peripheral oedema, and dry skin. Overall, the combination of dabrafenib and trametinib was found to provide an important treatment option for patients with BRAFV600E-mutant NSCLC.
REFERENCES
- Doebele RC et al., Mechanisms of resistance to crizotinib in patients with ALK gene rearranged non-small cell lung cancer. Clin Cancer Res 2012; 18: 1472-1482
- Zou HY et al., PF-06463922 is a potent and selective next-generation ROS1/ALK inhibitor capable of blocking crizotinib-resistant ROS1 mutations. PNAS 2015; 112: 3493-3498
- Nokihara H et al., Alectinib versus crizotinib in ALK inhibitor naïve ALK-positive non-small cell lung cancer: primary results from the JALEX study. J Clin Oncol 34, 2016 (suppl; abstr 9008) REFERENCES
- Kim D-W et al., Brigatinib in patients with crizotinib- refractory ALK+ non-small cell lung cancer: first report of efficacy and safety from a pivotal randomized phase 2 trial (ALTA). J Clin Oncol 34, 2016 (suppl; abstr 9007)
- Solomon BJ et al., Safety and efficacy of lorlatinib (PF-06463922) from the dose-escalation component of a study in patients with advanced ALK+ or ROS1+ non-small cell lung cancer (NSCLC). J Clin Oncol 34, 2016 (suppl; abstr 9009)
- Drilon AE et al., Antitumor activity and safety of crizotinib in patients with advanced MET exon 14-altered non-small cell lung cancer. J Clin Oncol 34, 2016 (suppl; abstr 108
- Planchard D et al., Dabrafenib in patients with BRAF(V600E)-positive advanced non-smallcell lung cancer: a single-arm, multicentre, open-label, phase 2 trial. Dabrafenib plus trametinib. Lancet Oncol 2016; 17(5): 642-650
- Planchard D et al., An open-label phase 2 trial of dabrafenib in combination with trametinib in patients with previously treated BRAF V600E– mutant advanced non-small cell lung cancer (BRF113928). J Clin Oncol 34, 2016 (suppl; abstr 107)
More posts
PFS improvement due to local therapy in oligometastatic NSCLC
Evidence suggests the existence of a ,limited metastatic’ NSCLC phenotype. However, the type of optimal treatment and the role of aggressive local therapy in these patients remain controversial. Gomez et al. presented the first prospective, randomised trial to address this question. Patients had stage IV disease without RECIST progression and a maximum of three metastases after front-line systemic therapy (FLST).
Locally advanced NSCLC: oral vinorelbine shows better safety profile than etoposide
The randomised, multicentre, open-label, phase II RENO trial was conducted with the objective of establishing a standard chemotherapy regimen in the setting of chemo-radiotherapy of locally advanced NSCLC. A total of 134 patients with inoperable stage III NSCLC received either oral vinorelbine plus cisplatin or etoposide plus cisplatin.
ULTIMATE: chemotherapy plus bevacizumab beyond first line
As chemotherapy in the second-line or third-line settings of NSCLC shows limited efficacy, the phase III, randomised ULTIMATE trial tested the combination of chemotherapy and bevacizumab in patients with advanced NSCLC of non-squamous histology, who had progressed after one or two lines of treatment.
New approaches are raising hope for SCLC patients
Only minor progress has been made over the past 30 to 40 years in the treatment of small-cell lung cancer (SCLC), which accounts for 10 % to 15 % of lung cancer cases. SCLC is radiosensitive, but approximately 70 % of patients present with extended disease that cannot be included within one radiotherapy field. The majority of patients respond to first-line chemotherapy.
Mutational analysis: on the road to refined standards
The Lung Cancer Mutation Consortium (LCMC) is a multi-institutional consortium for the study of driver mutations of lung adenocarcinoma. The cooperating sites enable the identification of relatively large numbers of patients with uncommon and rare alterations, facilitate the analysis of their clinical characteristics, and lay the ground for targeted therapy trials.
“The importance of first-line and second-line targeted agents is obvious”
Which parameters should be taken into consideration regarding the choice of EGFR TKIs in a lung cancer patient with an activating EGFR mutation? When EGFR mutations are diagnosed in the first-line setting, we have the luxury of having three options today. However, it is important to discriminate between the different types.