Different therapies for treatment of squamous cell carcinoma
Squamous cell carcinoma (SqCC) is one of the histopathological subtypes of non–small-cell lung cancer (NSCLC), and it accounts for 20 % to 30 % of these patients [1]. Unfortunately, few studies have explored the treatment options for patients with SqCC, and progress in SqCC treatment lags behind other histopathological and/or molecular subtypes of NSCLC [2]. At CSCO 2017, the main information relating to SqCC indicated that immunotherapies and targeted therapies do not provide satisfactory results. Additionally, the latest progress on afatinib for SqCC patients was reported.
Immunotherapies – hopeful prospect versus cruel reality?
The CheckMate 017 trial compared nivolumab to docetaxel as second-line treatment for SqCC patients, where nivolumab showed improved progression-free survival (PFS; 3.6 vs. 2.8 months; hazard ratio [HR] for death or disease progression, 0.62; 95 % confidence interval [CI], 0.47–0.81; p = 0.00004) and overall survival (OS; 9.2 vs. 6.0 months; HR, 0.59; 95 % CI, 0.44–0.79; p = 0.00025) compared to docetaxel [3]. The OAK trial compared atezolizumab to docetaxel as second-line or third-line treatment for SqCC patients, where atezolizumab also showed improved OS compared to docetaxel (8.9 vs. 7.7 months; p = 0.0383) [4].
Although these CheckMate 017 and OAK trials indicated promising results for immunotherapies as second-line treatments for SqCC patients, poor responses have been shown for SqCC patients treated with immunotherapies as first-line treatments. Govindan R et al. [5] conducted a phase III study to compare paclitaxel plus carboplatin in combination with ipilimumab (10 mg/kg) or placebo as first-line treatments for SqCC patients. However, no differences were seen between the two treatment groups for PFS (5.6 vs. 5.6 months) and OS (13.4 vs. 12.4 months; p = 0.25).
Thus, at CSCO 2017, Professor Qing Zhou from the Guangdong Lung Cancer Institute, Guangdong General Hospital and Guangdong Academy of Medical Sciences, Guangzhou (China) indicated that although immunotherapies have critical roles in the treatment of various cancers, they have shown little efficacy for treatment of SqCC patients [6].
Combining targeted therapy: multiple drugs, but poor benefit
According to the CSCO 2017 guidelines, the basic strategy for treatment of SqCC patients is platinum-based chemotherapy.
An EGFR-blocking antibody as first-line treatment of advanced SqCC
The SQUIRE trial compared the recombinant human IgG1 anti-EGFR monoclonal antibody necitumumab plus chemotherapy with chemotherapy alone, as first-line treatments for SqCC patients. Here the OS curves for necitumumab plus chemotherapy and chemotherapy alone almost overlapped. Although the absolute difference in OS was small (11.5 vs. 9.9 months; HR, 0.84; 95 % CI, 0.74–0.96; p = 0.01), this EGFR blocking antibody was approved by the US Food and Drug Administration as first-line treatment in advanced SqCC patients [7].
Afatinib as second-line treatment of advanced SqCC
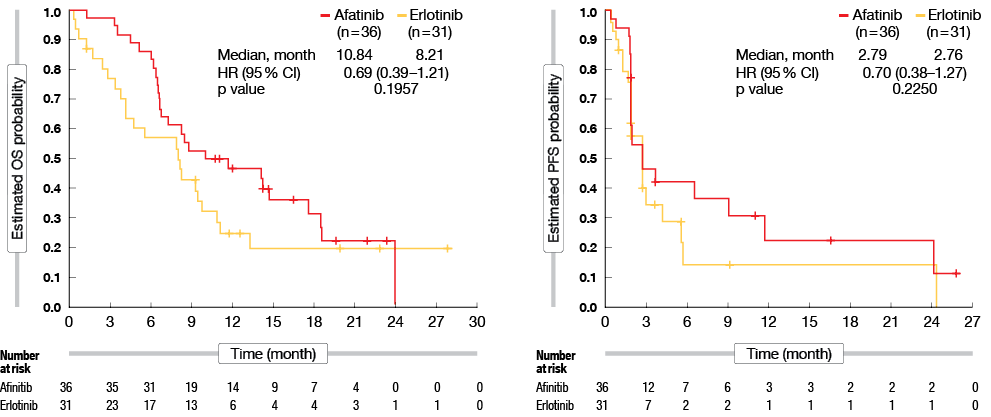
The LUX-Lung 8 trial compared afatinib to erlotinib as second-line treatment
in advanced SqCC patients. For all patients, afatinib showed greater improvements for PFS (2.6 vs. 1.9 months; HR, 0.81; 95 % CI, 0.69–0.96; p = 0.0103) and OS (7.9 vs. 6.8 months; HR, 0.81; 95 % CI, 0.69–0.95; p = 0.0077), compared to erlotinib [8]. In the updated subgroup analyses that focused on the Chinese patients, afatinib provided numerically greater PFS (2.79 vs. 2.76 months; p = 0.2250) and OS (10.84 vs. 8.21 months; p = 0.1957), compared to erlotinib (Figure 1) [9]. Although there was no significant superiority of afatinib over erlotinib in the Chinese subgroup, the Chinese guidelines for NSCLC treatment indeed recommend afatinib as second-line treatment for advanced SqCC.
In summary, although targeted therapies have not shown preponderant superiority as first-line or second-line treatments compared to the ‘traditional’ standard of care for SqCC patients, most organizations and countries have still focused on targeted therapies as the recommended treatment options for SqCC patients.
Figure 1: Estimated overall survival probability (left) and progression-free survival (right) with afatinib compared to erlotinib in the Chinese SqCC subgroup
Afatinib long-term responders
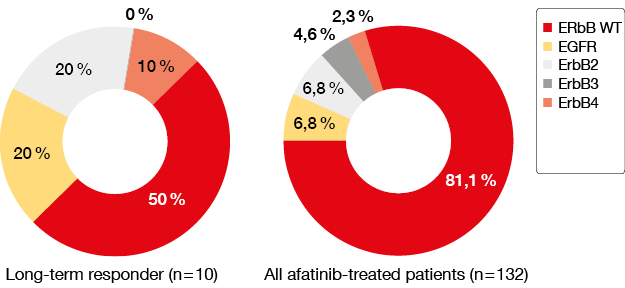
Additionally, a post-hoc analysis was reported from the LUX-Lung 8 trial, on the afatinib long-term responders (LTRs; with ≥ 12 months afatinib treatment). Here, 5 % of these SqCC patients were LTRs, with median PFS of 16.6 months and median OS of 21.1 months. The patient gene expression profiles obtained from next-generation sequencing were also compared between the LTRs and the rest of the afatinib-treated patients. ErbB-aberrations were more common in the LTRs than the overall afatinib-treated patients (Figure 2) [10]. Mass spectrometry analyses of the patient serum proteins using Veristrat also showed improvement for the LTRs compared to the overall afatinib-treated patients, in terms of those graded as Veristrat-good (88 % vs. 62 %). All of the patients who progressed received subsequent therapy, where 8/14 LTRs discontinued afatinib and received ≥1 subsequent line of systemic therapy, and 6/14 LTRs remained on afatinib at data cut-off; one of these patients received afatinib until death. Thus, the conclusion from this post-hoc analysis of afatinib LTRs was that after failing chemotherapy, 5 % of these SqCC patients were able to achieve long-term responses. The presence of ErbB-family mutations or Veristrat-good status might represent biomarkers of long-term responses to afatinib in advanced SqCC patients.
Figure 2: Comparison of ErbB-family variant mutations between long-term responders (left) and all afatinib-treated patients (right).
Afatinib plus cetuximab as second-line treatment of advanced SqCC
The unmet need for additional second-line treatments along with afatinib in advanced SqCC patients is still a clinical problem, and particularly for those with EGFR-T790M-mutant-negative tumors.
The EGFR inhibitor cetuximab has shown synergistic activity with afatinib in preclinical studies [11]. Data of a phase IB study of afatinib plus cetuximab were reported at CSCO 2017, as study 1 (S1; NCT01090011) in EGFR-mutant-positive NSCLC patients with resistance to gefitinib/ erlotinib (G/E), and Study 2 (S2; NCT02020577) in unselected patients with heavily pretreated advanced solid tumors, which included SqCC patients. In S1, these EGFR-mutant-positive NSCLC patients who were resistant to G/E were treated with afatinib (40 mg once daily) plus cetuximab (500 mg/m2 every 2 weeks). In S2, these patients with advanced solid tumors that included SqCC were treated with afatinib (40 mg once daily) plus cetuximab (250 mg/m2 weekly). In S1, the disease control rate (DCR) was 71 %, the median PFS was 4.7 months, and the discontinuation rate due to treatment-related adverse events was 13%. In S2, the overall DCR was 55%, but was higher for the SqCC patients, at 75 %. The median PFS was 11.9 weeks for the SqCC patients, and treatment-related adverse events occurred in 12 % of the total patient population, similar to that seen for study S1 [12]. The conclusion from these studies was that afatinib plus cetuximab provides benefits for EGFR-mutant-positive NSCLC patients who are resistant to G/E and for heavily pretreated SqCC patients, and that these benefits are accompanied by an acceptable safety profile.
On-going investigations into new targeted therapies
New targeted therapies for SqCC patients have been explored; however, most studies have not yielded the desired results. Studies on a fibroblast growth factor receptor inhibitor (dovitinib), a phosphoinositide 3-kinase inhibitor (pictilisib), a platelet-derived growth factor receptor inhibitor (motesanib) and a poly(adenosine diphosphate-ribose) polymerase inhibitor (iniparib) were all terminated early because of lack of efficacy or adverse events. The S1400 study was the first to be conducted through a government, academia, and pharma collaboration that focused on SqCC, which included the S1400B/C/D/E and S1400A/1 substudies for driver-oncogene-positive and -negative SqCC, respectively. The data from S1400B/C/D were presented at ASCO 2017, which compared the efficacies of GDC-0032 (phosphoinositide 3-kinase inhibitor), palbociclib (cyclin-dependent kinase 4/6 inhibitor) and AZD4547 (fibroblast growth factor receptor inhibitor) with docetaxel; however, these substudies were terminated early due to lack of efficacy.
Although the present situation is not favorable for new targeted therapies for SqCC patients, investigations into new potential therapies are still on-going, including those with an antisense oligonucleotide (apatorsen) and a cell-cycle blocker (abemaciclib). Professor Zhou thus indicated that although most studies of new therapies for SqCC patients have not been successful, the field is still moving forward [6].
REFERENCES
- Hirsh V et al., New Developments in the Treatment of Advanced Squamous Cell Lung Cancer: Focus on Afatinib. Onco Targets Ther. 2017;10:2513-2526.
- Schumacher TN et al., Neoantigens in Cancer Immunotherapy. Science. 2015;348(6230):69-74.
- Brahmer J et al., Nivolumab versus Docetaxel in Advanced Squamous-Cell Non–Small-Cell Lung Cancer. N Engl J Med. 2015;373:123-135.
- Rittermeyer A et al., Atezolizumab versus Docetaxel in Patients with Previously Treated Non–Small-Cell Lung Cancer (OAK): a Phase 3, Open-Label, Multicentre Randomised Controlled Trial. The Lancet. 2017;389(10066);255-265.
- Govindan R et al., Phase III Trial of Ipilimumab Combined With Paclitaxel and Carboplatin in Advanced Squamous Non–Small-Cell Lung Cancer. J Clin Oncol. 2017;35(30):3449-3457.
- Zhou Q et al., Progression and Challenge of SqCC. CSCO 2017.
- Thatcher N et al., Necitumumab plus Gemcitabine and Cisplatin versus Gemcitabine and Cisplatin Alone as First-Line Therapy in Patients with Stage IV Squamous Non–Small-Cell Lung Cancer (SQUIRE): an Open-Label, Randomised, Controlled Phase 3 Trial. Lancet Oncol. 2015;16(7):763-774.
- Soria JC et al., Afatinib versus Erlotinib as Second-Line Treatment of Patients with Advanced Squamous Cell Carcinoma of the Lung (LUX-Lung 8): an Open-Label Randomised Controlled Phase 3 Trial. Lancet Oncol. 2015;16(8):897-907.
- Lu S et al., Afatinib versus Erlotinib for Second-Line Treatment of Chinese Patients with Advanced Squamous Cell Carcinoma of the Lung: a Subgroup Analysis of the Phase III LUX-Lung 8 Trial. CSCO 2017.
- Lu S et al., Post-hoc Analysis of Afatinib Long-Term Responders in the Phase III LUX-Lung 8 Trial in Patients with Advanced Squamous Cell Carcinoma of the Lung. CSCO 2017.
- Regales L et al., Dual Targeting of EGFR Can Overcome a Major Drug Resistance Mutation in Mouse Models of EGFR Mutant Lung Cancer. J Clin Invest. 2009;119(10):3000-3010.
- Charles J et al., The Story of Afatinib plus Cetuximab in the Treatment of Patients with NSCLC to Date. CSCO 2017.
More posts
Determination of clinical responses to immunotherapy
In the past 13 years, an earthshaking change has occurred in treatment of non–small-cell lung cancer (NSCLC). The emergence of two new treatment methods – targeted treatment and immunotherapy – has overturned doctors’ and patients’ perception of standard of care for NSCLC. However, not all of the driver oncogenes in NSCLC have been identified.
New insights into the treatment of ALK-mutant-positive NSCLC patients
Anaplastic lymphoma kinase (ALK) is a fusion oncogene, and the prevalence of ALK mutations in NSCLC patients is similar across different races. At CSCO 2017, the main progress for the treatment of ALK-mutant-positive NSCLC patients related to the new recommendations for first-line and second-line treatments, and the optimal strategies to manage patients before and after resistance to ALK tyrosine kinase inhibitors (TKIs).
Optimal strategy for the treatment of EGFR-mutant lung cancer
The emergence of EGFR TKIs has changed the standard of care in EGFR-mutant NSCLC patients. IPASS was the first open-label randomized study to compare the first-generation EGFR TKI gefitinib with platinum-based chemotherapy in Chinese patients with EGFR-mutant NSCLC. It showed that the disease-free survival (DFS) rate was remarkably higher in the gefitinib group compared to chemotherapy.
Different therapies for treatment of squamous cell carcinoma
Squamous cell carcinoma (SqCC) is one of the histopathological subtypes of non–small-cell lung cancer (NSCLC), and it accounts for 20 % to 30 % of these patients [1]. Unfortunately, few studies have explored the treatment options for patients with SqCC, and progress in SqCC treatment lags behind other histopathological and/or molecular subtypes of NSCLC [2].
Diagnosis of EGFR-mutated NSCLC: from guidelines to reality
Over the last decade, the increasing understanding of critical molecular and cellular mechanisms which drive tumor initiation, maintenance, and progression in non-small-cell lung cancer (NSCLC) have contributed to the discovery of various novel drug targets and the development of new treatment strategies.
Guidelines for the treatment of NSCLC in China: progress and controversies
Lung cancer (LC) is the leading cause of tumor deaths worldwide. Per year, 1.8 million people are diagnosed with LC, and the annual death toll amounts to 1.6 million. Non–small-cell lung cancer (NSCLC) is the most common type, which accounts for 85% of LC cases. Squamous cell carcinoma (SqCC), adenocarcinoma (AC), and large-cell carcinoma are subtypes of NSCLC.