Early-stage NSCLC: promising (neo)adjuvant approaches
The NEOSTAR trial
Effective treatment options are called for in patients with resectable non-small-cell lung cancer (NSCLC), as more than half of those with stage I to III disease experience relapses [1]. Chen et al. demonstrated in their animal model that tumor PD-L1 upregulation is critical for the spread and survival of metastases [2]. Based on these considerations, several clinical trials are investigating the potential benefits of immunotherapies in the neoadjuvant setting.
The randomized phase II NEOSTAR trial included 44 surgical candidates with stage I to IIIA NSCLC [3]. They were randomized to 3 doses of nivolumab 3 mg/kg on days 1, 15, and 29, or the same nivolumab schedule plus ipilimumab 1 mg/kg on day 1. Surgery was performed within 3 to 6 weeks after the last dose. Major pathological response (MPR), i.e., ≤ 10 % viable tumor cells, was defined as the primary endpoint. It was assumed that nivolumab and/or the combination will produce an MPR rate greater than the one achieved with induction chemotherapy as compared to historical controls. Among the 44 randomized patients, who made up the intent-to-treat (ITT) population, 23 received nivolumab alone, and 21 were treated with nivolumab plus ipilimumab. Thirty-nine patients underwent surgical resection.
Clinical benefits & increased T-cell infiltration
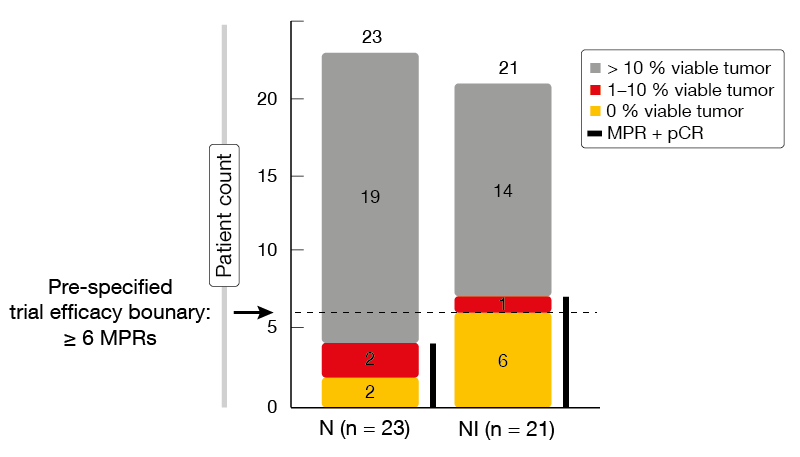
The MPR rate observed in the combination group met the pre-specified trial efficacy boundary. For the ITT population, it was shown that MPRs plus pathological complete responses (pCRs; i.e., 0 % viable tumor cells) occurred in 33 % of patients treated with both nivolumab and ipilimumab (Figure 1). With nivolumab alone, this was 17 %. In the resected population, the combination induced a 44 % MPR plus pCR rate, with pCR accounting for 38 % (MPR plus pCR for nivolumab, 19 %). Overall response rates (ORR) by RECIST according to imaging were 19 % and 22 %, respectively, in the ITT population. One patient in the combination arm (5 %) achieved complete response (CR); in both arms, a total of eight patients (36 %) had partial responses (PRs).
No unacceptable toxicity or increases of perioperative morbidity or mortality were observed. However, the authors noted that nodal immune flares deserve attention in the context of neoadjuvant immunotherapy, as patients might experience seeming radiographic nodal progression due to the emergence of granulomas that need to be distinguished from tumor growth. This is important as potentially curative surgery might be withheld if clinicians fail to differentiate between nodal immune flares and disease progression.
RECIST responses were shown to be positively associated with MPR rates. Elevated baseline PD-L1 expression correlated with radiographic responses and pathological tumor regression. In accordance with the improvement of response rates, immune characterization of surgical samples by flow cytometry revealed that the combined treatment was associated with higher frequencies of CD3-positive tumor-infiltrating lymphocytes as well as tissue resident and effector memory T cells. Moreover, nivolumab plus ipilimumab gave rise to increases of T cell repertoire diversity and reactivity in the tumor.
Figure 1: NEOSTAR: pathological response rates obtained with
Single-agent atezolizumab: LCMC3
The multicenter phase II LCMC3 study is currently assessing the PD-L1 inhibitor atezolizumab in patients with stage IB, II, IIIA and selected IIIB resectable and untreated NSCLC (planned accrual, n = 180). Two cycles of atezolizumab are administered prior to surgery. MPR constitutes the primary endpoint. At the ASCO 2019 Congress, Kwiatkowski et al. presented the results of the efficacy interim analysis [4]. At this time, the safety population comprised 101 patients. Among these, 90 (89 %) underwent surgery and thus represented the intended surgery population. Eighty-four resected patients (83 %) had MPR assessment. After the exclusion of patients with EGFR– and ALK-positive tumors, the primary efficacy population included 77 individuals (76 %). As many as 46 % of the patients in the safety population had stage IIIA/IIIB disease, and 51 % showed PD-L1 expression.
In the intended surgery population, PR and disease stabilization (SD) were achieved in 7 % and 89 %, respectively. For the primary efficacy population, the MPR rate amounted to 19 %, and 5 % of patients obtained pCRs. Forty-nine percent had ≥ 50 % pathological regression of their specimens. The authors rated these results as encouraging considering the advanced stage of disease in a large proportion of patients. Pathological regression correlated moderately with changes in tumor lesion size according to RECIST. MPR and pathological regression occurred irrespective of PD-L1 expression and tumor mutational burden. Moreover, no significant associations between gene alterations and MPR were observed. Atezolizumab monotherapy was well tolerated, and no new safety signals emerged. As this interim analysis passed its futility boundary, study enrollment continues. IMpower030, a placebo-controlled phase III study investigating atezolizumab combined with platinum-based chemotherapy, is ongoing.
Chemo-immunotherapy: pCR of 71 %
A combined neoadjuvant approach was tested by the multicenter, single-arm, open-label phase II NADIM study [5]. Patients with resectable stage IIIA NSCLC received 3 cycles of nivolumab 360 mg plus chemotherapy with paclitaxel and carboplatin. Surgery was performed in the third or fourth week after day 21 of the third cycle. Thereafter, adjuvant treatment consisting of nivolumab was administered for a total of one year. The ITT population consisted of 46 patients, with 41 undergoing surgery.
Nivolumab plus chemotherapy proved tolerable. None of the patients withdrew from the study preoperatively due to disease progression or toxicity, and surgery was not delayed in any patient. No intraoperative complications occurred, and postoperative complications were manageable. Neoadjuvant treatment resulted in clinical responses in almost all of the patients. The CR and PR rates amounted to 6.5 % and 72 %, respectively, and SD was observed in 17.5 %. Major pathological responses occurred in 85.36 %. At 71.4 %, the pCR rate was unprecedented. Down-staging was obtained in 93 % of cases.
JIPANG: adjuvant pemetrexed proves feasible
In the setting of postoperative adjuvant chemotherapy, the randomized JIPANG trial attempted to answer the question of which cisplatin-based regimen is most effective [6]. Patients with completely resected non-squamous stage II to IIIA NSCLC were randomized to either pemetrexed plus cisplatin (n = 389) or vinorelbine plus cisplatin (n = 395). Each regimen was administered for up to 4 cycles. JIPANG was the first phase III trial to assess pemetrexed plus cisplatin as a postoperative adjuvant regimen.
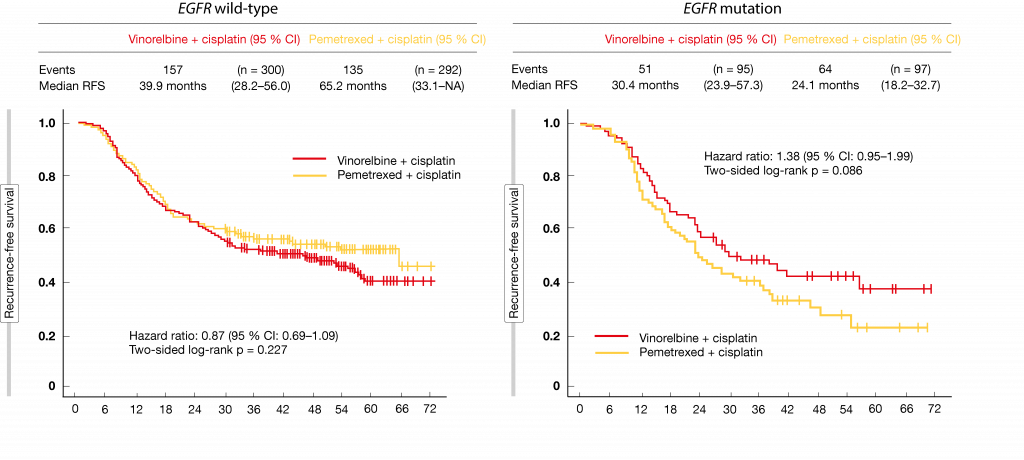
For recurrence-free survival (RFS), which was defined as the primary endpoint, the trial showed no superiority of pemetrexed plus cisplatin. However, the two regimens demonstrated similar efficacy (median RFS, 38.9 vs. 37.3 months with pemetrexed plus cisplatin vs. vinorelbine plus cisplatin; HR, 0.98). Similarly, OS did not differ across the arms (HR, 0.98). The RFS-related subgroup analysis suggested that patients with EGFR mutations fared better with the vinorelbine regimen, while those with EGFR wild-type derived greater benefit from the pemetrexed-based treatment (Figure 2).
Figure 2: Greater relapse-free survival benefit with pemetrexed plus cisplatin in EGFR wild-type patients, and with vinorelbine plus cisplatin in patients with EGFR mutations
At the same time, pemetrexed plus cisplatin showed higher tolerability. A greater proportion of patients completed 4 cycles of treatment (87.9 % vs. 72.7 %), and toxicity was milder, with lower rates of serious and grade 3 to 5 adverse events (AEs). Severe hematological AEs occurred significantly less frequently (24.7 % vs. 81.8 %; p < 0.001), and the treatment discontinuation rate was lower (9.5 % vs. 23.5 %). Based on these data, pemetrexed plus cisplatin can be an option for postoperative adjuvant chemotherapy in stage II to IIIA non-squamous NSCLC, especially for patients with EGFR wild-type disease.
Postoperative EGFR TKI treatment
The role of adjuvant EGFR tyrosine kinase inhibitor (TKI) therapy in early-stage EGFR-mutant NSCLC is still controversial. In their meta-analysis of 11 trials including a total of 1,152 resected NSCLC patients with activating EGFR mutations, Tang et al. found that when compared to treatment without adjuvant EGFR TKIs, EGFR TKIs prolonged both OS (OR, 0.63; p = 0.004) and disease-free survival (DFS; OR, 0.56; p < 0.00001) [7]. Predefined subgroup analyses suggested a greater DFS benefit with EGFR TKIs than with chemotherapy. However, this did not apply to OS. Compared to chemotherapy alone, the combination of EGFR TKI treatment and chemotherapy resulted in significantly longer DFS (OR, 0.48; p < 0.00001) and OS (OR, 0.50; p = 0.003). In addition, TKI-treated patients showed fewer grade ≥ 3 AEs than the chemotherapy-treated cohorts (OR, 0.22; p < 0.00001). Considering these findings, adjuvant EGFR TKIs are a potential treatment option as single agents or combined with chemotherapy in patients with completely resected EGFR-positive NSCLC.
Alterations of the tumor microenvironment (TME) might help inform patient selection with respect to adjuvant EGFR TKI treatment. Khalil et al. identified 8 key TME genes whose high expression was associated with improved DFS in patients with EGFR mutations [8]. The researchers clustered them in two groups characterized by distinct immune profiles. One group showed a more “inflamed” phenotype (e. g., higher lymphocyte infiltration score and TGF-β response) than the other. Both DFS and disease-specific survival were significantly longer in the inflamed group than in the non-inflamed group. The results suggest that patient stratification according to these genes could contribute to identifying individuals who will benefit from adjuvant therapy.
Three months vs. 2 years of afatinib
As the optimal duration of adjuvant EGFR TKI treatment is under debate, a randomized phase II trial assessed the daily administration of afatinib for 2 years (n = 22) versus 3 months (n = 24) in patients who had completed standard adjuvant treatment after resection of stage I to III NSCLC [9]. The study was closed at 46 of 60 planned patients for slow accrual. DFS at 2 years was defined as the primary endpoint. Here, the 2-year regimen induced a 14 % reduction of recurrence rates compared to the 3-month schedule (DFS at 2 years, 85 % vs. 71 %), although this difference was not statistically different. Median DFS and OS have not been reached in either arm yet.
As in prior trials of adjuvant EGFR TKIs, many patients in the 2-year arm did not complete treatment, with withdrawal of consent being the main reason (23 %), followed by toxicity (18 %) and recurrence (9 %). The authors concluded that in the era of TKIs with improved tolerance, the duration of adjuvant therapy remains an important question.
Personalization of consolidation immunotherapy
Moding et al. investigated the use of circulating tumor DNA (ctDNA) for the detection of molecular residual disease after chemoradiation therapy (CRT) in patients with localized NSCLC [10]. The scientists hypothesized that consolidation immune checkpoint inhibition (CICI) after CRT, which gives rise to additional toxicity and costs, might be omitted in patients with undetectable ctDNA. Samples were collected from 62 patients with stage IIB to IIIB NSCLC who received concurrent CRT with curative intent. CICI was administered in 25 of these.
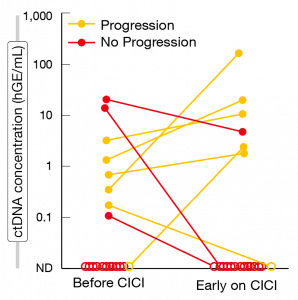
Indeed, the presence of ctDNA was shown to have predictive power. In the group without detectable ctDNA after CRT, median freedom from progression (FFP) had not been reached yet at the time of analysis; these patients have an excellent prognosis and might not benefit from CICI. Reassessments during the early CICI phase demonstrated that ctDNA changes might identify responders and non-responders to consolidation therapy. Median FFP had not been reached yet in patients without detectable ctDNA during early CICI. In those who showed ctDNA decreases, median FFP was 16.5 months; this group did not experience progression and thus appeared to benefit from immunotherapy (Figure 3). Patients who had ctDNA increases after the start of consolidation fared worst, with a median FFP of 0.4 months. Here, rapid progression indicated a lack of response to treatment.
The authors proposed an algorithm including the initiation of CICI after CRT only if ctDNA is present. Early after the start of CICI, another analysis would be conducted that prompts either a change in treatment or the continuation of immunotherapy depending on the persistence of ctDNA. Patients who do not show detectable ctDNA after CRT would not receive CICI but undergo ctDNA surveillance in addition to imaging. Nevertheless, prospective clinical trials will be essential to establish the ability of the ctDNA analysis to personalize consolidation immunotherapy.
Figure 3: Association between changes in ctDNA levels and clinical course in patients receiving immune checkpoint inhibitor consolidation (CICI) after adjuvant chemoradiation.
REFERENCES
- Pignon JP et al., Lung adjuvant cisplatin evaluation: a pooled analysis by the LACE Collaborative Group. J Clin Oncol 2008; 26(21): 3552-3559
- Chen L et al., Metastasis is regulated via microRNA-200/ZEB1 axis control of tumour cell PD-L1 expression and intratumoral immunosuppression. Nat Commun 2014; 5: 5241
- Cascone T et al., Neoadjuvant nivolumab or nivolumab plus ipilimumab for resectable non-small cell lung cancer (NSCLC): clinical and correlative results from the NEOSTAR study. J Clin Oncol 37, 2019 (suppl; abstr 8504)
- Kwiatkowski DJ et al., Neoadjuvant atezolizumab in resectable non-small cell lung cancer (NSCLC): interim analysis and biomarker data from a multicenter study (LCMC3). J Clin Oncol 37, 2019 (suppl; abstr 8503)
- Provencio M et al., Neo-adjuvant chemo-immunotherapy for the treatment of stage IIIA resectable non-small-cell lung cancer (NSCLC): a phase II multicenter exploratory study. Final data of patients who underwent surgical assessment (NADIM). J Clin Oncol 37, 2019 (suppl; abstr 8509)
- Kenmotsu H et al., Randomized phase III study of pemetrexed/cisplatin versus vinorelbine/cisplatin for completely resected non-squamous non-small-cell lung cancer. The JIPANG study. J Clin Oncol 37, 2019 (suppl; abstr 8501)
- Tang W et al., EGFR inhibitors as adjuvant therapy for EGFR mutation positive non-small cell lung cancer. J Clin Oncol 37, 2019 (suppl; abstr 8508)
- Khalil M et al., The tumor microenvironment in EGFR-driven loco-regional lung adenocarcinoma can predict higher risk of recurrence. J Clin Oncol 37, 2019 (suppl; abstr 8521)
- Chaft JE et al., Randomized phase II study of adjuvant afatinib for 3 months versus 2 years in patients with resected stage I-III EGFR mutant NSCLC. J Clin Oncol 37, 2019 (suppl; abstr 8507)
- Moding EJ et al., ctDNA for personalization of consolidation immunotherapy in localized non-small cell lung cancer. J Clin Oncol 37, 2019 (suppl; abstr 2547)
© 2019 Springer-Verlag GmbH, Impressum