Checkpoint inhibition: predictors, resistance and immunogenomic features
Predictors of immunotoxicity to checkpoint inhibitors
Immune checkpoints, such as cytotoxic T-lymphocyte associated protein-4 (CTLA-4) or programmed cell death protein 1 (PD-1), downregulate T-cell responses and are crucial for self-tolerance, which protects the body against attacking cells indiscriminately [1]. Tumor cells hijack this mechanism to evade the immune However, specific immune-related adverse events (irAEs) have been described in various clinical trials [2, 4]. There is an unmet need to identify predictive biomarkers to anticipate patients’ susceptibility to irAEs [5]. So far, data specifically linking the tumor immune response to the risk of experiencing irAEs are scarce [6].
The analyzed population included 472 patients with various cancer entities who had tumor immune profiling performed on paraffin embedded formalin fixed archival tumor samples using the omniseq immune report card [6]. The patients subsequently underwent CPI therapy. The immune report card enclosed the enumeration of tumor infiltrating lymphocytes (TILs) by immunohistochemistry (IHC) and TIL-associated genes by RNA-sequencing, programmed cell death 1 ligand 1 (PD-L1) expression via IHC, and tumor mutational burden (TMB) via DNA-sequencing. The irAEs (type and grade) were investigated based on retrospective patient chart review, and their association with immune biomarkers analyzed statistically.
More than half of the patients had lung cancer (55 %), 9 % ovarian cancer, and 6 % melanoma. The median age of the patients was 61 (range, 53-70) and 56 % were women. Most of the patients received an anti-PD-1/PD-L1 treatment (94 %), while 6 % had a combination therapy. Among the 37 % of patients who developed irAEs, 3 % had grade ≥3 irAEs. The most affected organs were the skin (11 %), thyroid gland (10 %), and gastrointestinal tract (9 %).
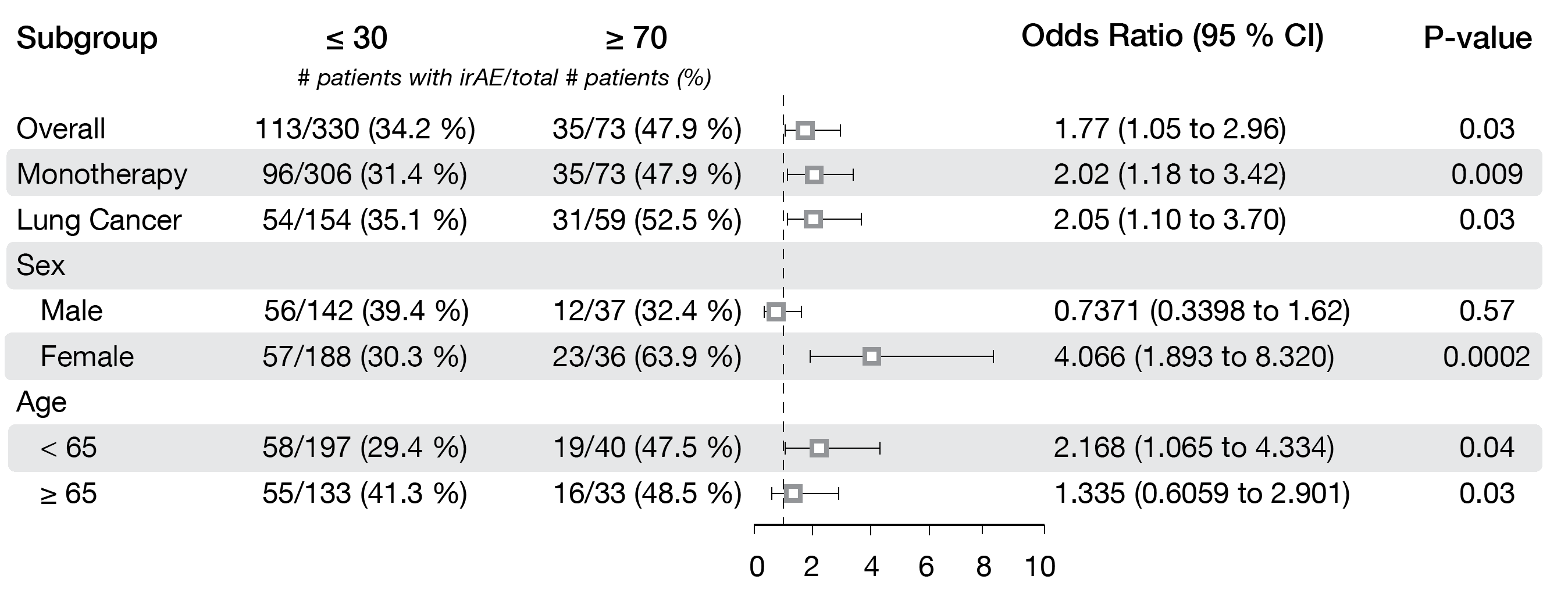
An increased number of TILs was associated with a high risk for any irAEs (p = 0.04; OR, 1.74, 95 % CI: 1.03-2.93), but only in males (p = 0.006; OR, 3.60; 95 % CI, 1.38-8.96). Patients who had PD-1/PD-L1 monotherapy and/or lung cancer showed a strong association (p = 0.02; OR, 1.99; 95 % CI: 1.12-3.41 and p = 0.01; OR, 2.36; 95 % CI: 1.21-4.61, respectively). A significant relation between a high PD-L1 expression – defined as >70 % via IHC – and an increased risk for any irAEs (p = 0.03; OR, 1.77, 95 % CI: 1.05-2.96] was also observed (Figure 1). Women (p = 0.0002; OR, 4.07; 95 % CI: 1.89-8.32) and patients <65 years (p = 0.04; OR, 2.17; 95 % CI: 1.07-4.33) revealed to have a high risk to develop irAEs. A high TMB expression was not associated with a more elevated risk for irAEs, except in the female population (p = 0.01) or in breast cancer patients (p = 0.03).
The study demonstrated a correlation between the tumor immune environment and the immune toxicity, as increased TILs and a high PD-L1 expression were associated with an elevated risk for irAEs in patients receiving immunotherapy.
Figure 1: Association between PD-L1 expression and risk for irAEs
immunotherapy has been previously shown to improve CPI response rates [9, 10].
immune response. In preclinical settings, this radioenhancer showed antitumor efficacy in various tumors; especially in the combination NBTXR3 plus radiation therapy, a local and a systemic control, as well as an induction of the immune response, were observed in mice [11-13]. Moreover, in in vivo tumor ents with locally advanced head and neck squamous cell carcinoma (HNSCC) who are not eligible for a platinum-based chemotherapy [15-17]. New data recently presented at ASCO 2021 showed that NBTXR3 activated through radiation acts synergistically with anti-PD-1 therapy to enhance the therapeutic index of the RT and to overcome PD-1 resistance [14, 18].
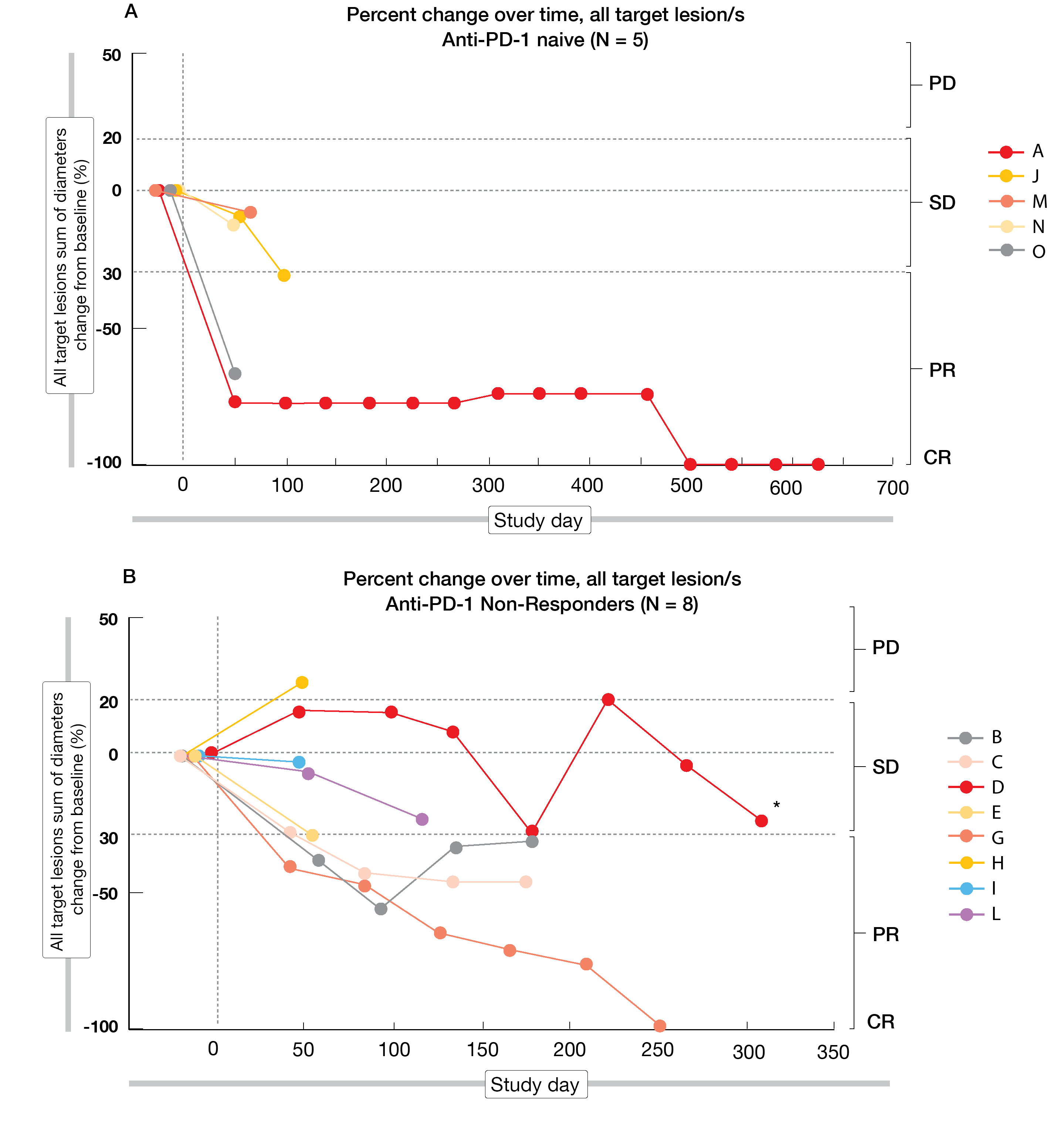
An ongoing multicenter, open-label, non-randomized, phase I, first-in-human study evaluates the safety and tolerability of RT-activated NBTXR3 in combination with anti-PD-1 in three cohorts. The first cohort includes patients with locoregional recurrent (LRR) or recurrent and metastatic (R/M) HNSCC at the target lesion in a previously irradiated field. In cohort 2 and 3, patients with respectively lung or liver metastases from any primary cancer eligible for anti-PD-1 treatment are enrolled [14, 18]. About 60 patients will receive RT-activated NBTXR3 in combination with an approved anti-PD-1 therapy (NCT03589339). Primary endpoints enclose the determination of the recommended phase 2 dose, dose limiting toxicities and maximum tolerated dose. Secondary objectives include antitumor response (objective response rate by RECIST 1.1), safety, and feasibility of the NBTXR3 injection. First results demonstrated tumor regression in 10 out of 13 patients evaluable for tumor responses, regardless of prior anti-PD-1 exposure [14]. Four out of five anti-PD-1 naïve patients experienced a regression; ORR reached 60 %, including one complete response (CR) (Figure 2A). In anti-PD-1 non-responders, 78 % (n = 6) had post-treatment tumor regression and ORR was 50 % (1 CR and 2 partial responses) (Figure 2B). Altogether, among 16 serious adverse events (SAE) observed, four were related to NBTXR3 or injection related, and included hyperglycemia, pneumonitis, and soft tissue necrosis.
Taken together, this data underline the immune modulation effect of radiotherapy-activated NBTXR3, not only as single agent, but also in combination with an anti-PD-1 treatment.
Figure 2 A, B: Change over time related to baseline in tumor size stratified by anti-PD-1 status
* Patient D: partial complete response based on biopsy sample located in the target lesion
Neoadjuvant immunotherapy effect on tumor microenvironment
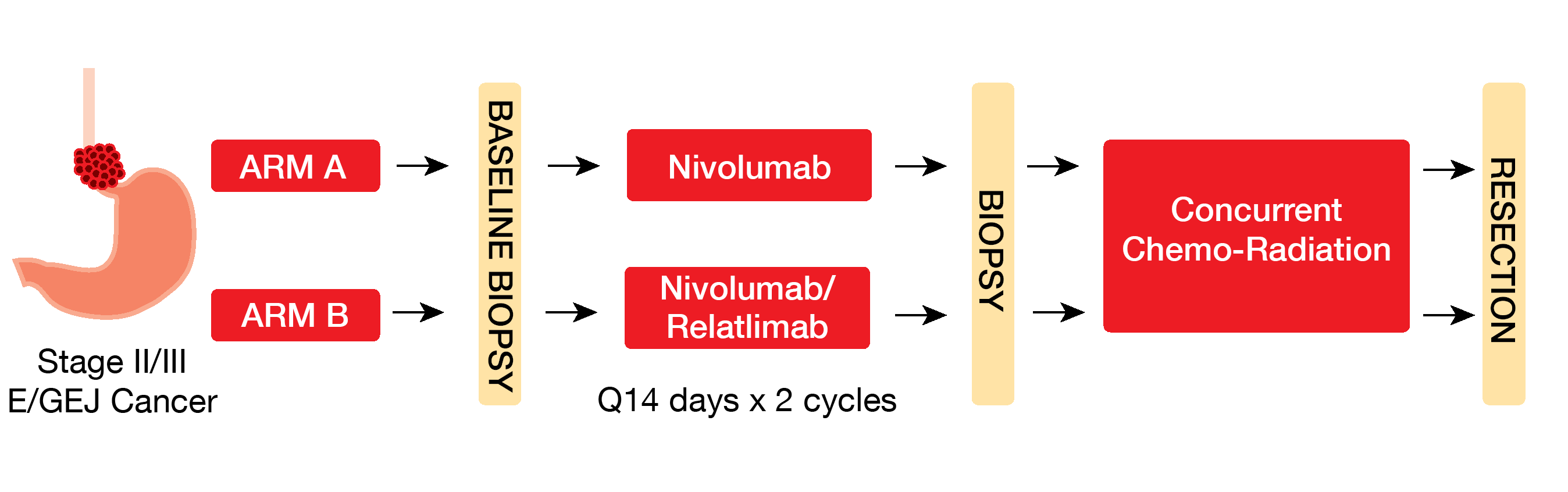
In patients with resectable esophageal or gastroesophageal junction (E/GEJ) cancer, the standard-of-care neoadjuvant chemoradiation is associated with a high recurrence rate [20]. In the CheckMate 577 trial, the treatment with the CPI nivolumab as adjuvant therapy following neoadjuvant chemoradiation and surgery s checkpoint blockade therapy [22, 23]. This phase IB study assessed the safety of two cycles anti-PD-1 nivolumab alone or nivolumab plus the anti-LAG3 relatlimab with chemoradiation in the preoperative setting (NCT03044613). Serial tumor samples from 23 patients were collected prior to therapy, after two cycles of CPI induction, and at resection (Figure 3). Pathologic response was measured by tumor regression at resection. Median follow up was 23 months post-surgery. Overall, 48 serial tumor samples were analyzed via bulk RNA sequencing (RNAseq), while 22 baseline tumor and normal DNA pairs were analyzed by whole exome sequencing (WES) to find somatic mutations and generate tumor mutation burden (TMB) estimates.
After immunotherapy induction, a significant upregulation of interferon-alpha (IFN-α), interferon-gamma (IFN-γ), tumor-necrosis factor-α (TNF-α) and antigen presentation related genes were detected compared to baseline (p<0.0001). On the other hand, E2F targets (p = 0.002), G2M checkpoint genes (p = 0.005) and DNA damage repair genes (p = 0.004) were significantly downregulated following CPI neoadjuvant treatment. Patients who reached a pathologic complete response (pCR) were those whose tumors harbored a high number of expressed mutations (p = 0.026). A significantly higher density of intratumoral activated M1 macrophages was observed post-induction with CPI in patients with pCR (p = 0.0034). Additionally, TMB was not a predictive marker of a pathologic response (p = 0.22).
In summary, CPI neoadjuvant therapy induced an inflammatory immune response in the tumor microenvironment which was associated with tumor elimination and pathologic response.
Figure 3: Study design, including sample collection timeline
REFERENCES
- Li B et al., Immune Checkpoint Inhibitors: Basics and Challenges. Curr Med Chem 2019; 26(17): 3009-3025.
- Baxi S et al., Immune-related adverse events for anti-PD-1 and anti-PD-L1 drugs: systematic review and meta-analysis. Bmj 2018; 360: k793.
- Tray N et al., Predictive Biomarkers for Checkpoint Immunotherapy: Current Status and Challenges for Clinical Application. Cancer Immunol Res 2018; 6(10): 1122-1128.
- Ramos-Casals M et al., Immune-related adverse events of checkpoint inhibitors. Nat Rev Dis Primers 2020; 6(1): 38.
- Gibney GT et al., Predictive biomarkers for checkpoint inhibitor-based immunotherapy. Lancet Oncol 2016; 17(12): e542-e551.
- Alexander W et al., Using the tumor microenvironment to identify predictors of immunotoxicity to checkpoint inhibitors. J Clin Oncol 2021; 39(suppl 15; abstr 2545).
- Schoenfeld AJ et al., Acquired Resistance to Immune Checkpoint Inhibitors. Cancer Cell 2020; 37(4): 443-455.
- Sharma P et al., Immune checkpoint targeting in cancer therapy: toward combination strategies with curative potential. Cell 2015; 161(2): 205-14.
- Hwang WL et al., Safety of combining radiotherapy with immune-checkpoint inhibition. Nat Rev Clin Oncol 2018; 15(8): 477-494.
- Postow MA et al., Immunologic correlates of the abscopal effect in a patient with melanoma. N Engl J Med 2012; 366(10): 925-31.
- Maggiorella L et al., Nanoscale radiotherapy with hafnium oxide nanoparticles. Future Oncol 2012; 8(9): 1167-81.
- Marill J et al., Hafnium oxide nanoparticles: toward an in vitro predictive biological effect? Radiat Oncol 2014; 9: 150.
- Zhang P et al., Radiotherapy-Activated Hafnium Oxide Nanoparticles Produce Abscopal Effect in a Mouse Colorectal Cancer Model. Int J Nanomedicine 2020; 15: 3843-3850.
- Seiwert TY et al., Overcoming resistance to anti-PD-1 with tumor agnostic NBTXR3: From bench to bed side. J Clin Oncol 2021; 39(suppl 15; abstr 2591).
- Anselmo AC et al., Nanoparticles in the clinic: An update. Bioeng Transl Med 2019; 4(3): e10143.
- Bonvalot S et al., NBTXR3, a first-in-class radioenhancer hafnium oxide nanoparticle, plus radiotherapy versus radiotherapy alone in patients with locally advanced soft-tissue sarcoma (Act.In.Sarc): a multicentre, phase 2-3, randomised, controlled trial. Lancet Oncol 2019; 20(8): 1148-1159.
- Hoffmann C et al., Phase I dose-escalation study of NBTXR3 activated by intensity-modulated radiation therapy in elderly patients with locally advanced squamous cell carcinoma of the oral cavity or oropharynx. Eur J Cancer 2021; 146: 135-144.
- Shen C et al., A phase I trial evaluating NBTXR3 activated by radiotherapy in combination with nivolumab or pembrolizumab in patients with advanced cancers. J Clin Oncol 2021; 39(15_suppl; abstr 2590).
- Baere TD Phase I/II Study Of Radiation Enhancing Hafnium Oxide Nanoparticles NBTXR3 Activated by SBRT in HCC and Liver Metastases Patients. international journal of radiation oncology, biology, physics 2020; 108(3).
- Blum Murphy M et al., Pathological complete response in patients with esophageal cancer after the trimodality approach: The association with baseline variables and survival-The University of Texas MD Anderson Cancer Center experience. Cancer 2017; 123(21): 4106-4113.
- Kelly RJ et al., Adjuvant Nivolumab in Resected Esophageal or Gastroesophageal Junction Cancer. N Engl J Med 2021; 384(13): 1191-1203.
- Anagnostou V et al., Multimodal genomic features predict outcome of immune checkpoint blockade in non-small-cell lung cancer. Nat Cancer 2020; 1(1): 99-111.
- Belcaid Z et al., Immunogenomic features of pathologic response to neoadjuvant immune checkpoint blockade in esophageal cancer. J Clin Oncol 2021; 39(suppl 15; abstr 4042).
© 2021 Springer-Verlag GmbH, Impressum